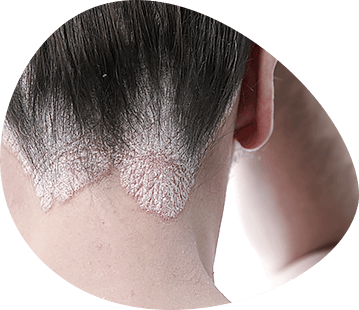
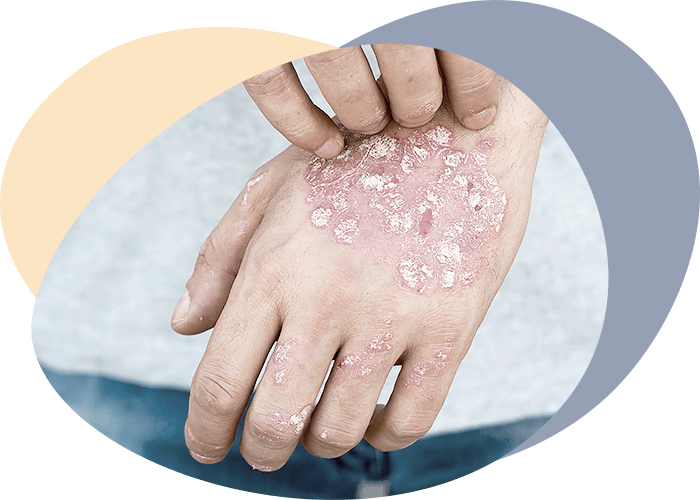
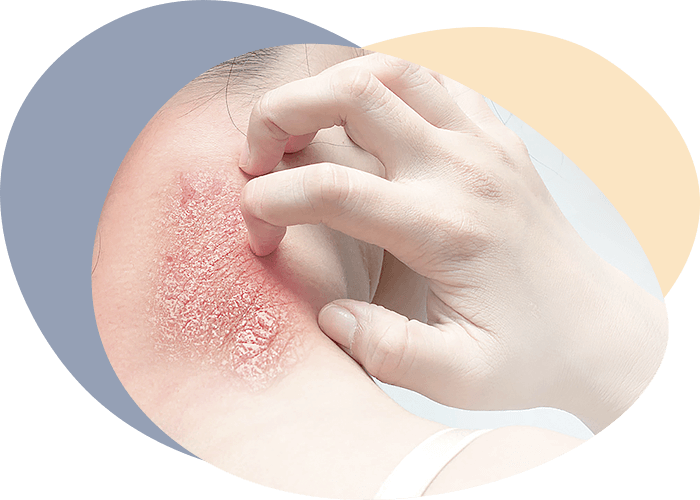
Many people underestimate the importance of skin, considering it just a human shell, but it performs a number of indispensable functions in the body. First of all, skin is a barrier to penetration into the body, as pathogens, and a large number of harmful substances. It is the barrier to the penetration of solar radiation into the body - the main cause of aging and malignant cell regeneration. It acts as a thermoregulation, preventing overheating and overcooling.
The skin is the excretion organ. Through pores, with sweat, a large number of hazardous substances are removed from the body. For example, the concentration of heavy metal salts in sweat is highest, which means that heavy metals are mainly removed from the body by the skin. Skin takes part in fat, carbohydrate and salt metabolism. Vitamin D is synthesized in the skin. It is safe to say that it is the mirror of human health, habits, age, diet and lifestyle. It is in connection with its many functions and a large number of skin diseases.
Skin. Its structure and functions
Skin - the external cover of the body, protecting the body from a wide range of external influences, participating in breathing, thermal regulation, exchange and many other processes. In addition, the skin is a massive receptor field of various types of surface sensitivity. Skin consists of epidermis, dermis and subcutaneous fatty tissue (hypodermis).
Distinguishing:
- thick skin (palms and soles) - formed by a thick (400-600 microns) epidermis, no hair and sebaceous glands;
- fine skin (on the rest of the body) - consists of a thin (70-140 microns) epidermis; there are no hair and sebaceous glands.
Functions of the skin:
- protective (barrier) protects the body from mechanical and chemical factors, UV radiation, microbial penetration, loss and ingress of water from the outside.
- radiant heat and sweat
- participation in water-salt exchange is associated with sweating
- excretion of metabolic products, salts and drugs
- endocrine and metabolic synthesis and accumulation of vitamin D as well as hormones
- sensory (provides a sense of heat and cold, touch, pain)
- immune capture, processing and transport of antigens with subsequent development of the immune response,
- respiration
Age-related skin changes
In the process of human life, the skin changes. In a small child, it is thin, gentle, easily vulnerable. The epidermis is much thinner than an adult, the corneal layer is poorly developed. At the same time, the subcutaneous fatty tissue in the child is thicker. In children, the skin is supplied with blood more abundantly, its vessels are dilated, the permeability of the vessel walls is increased. All this predisposes to inflammation with swelling, bubbles, bubbles. Thermoregulation and sweating in children are imperfect, they easily overheat, sweat, in this regard, especially with poor care, they easily develop sweating, intertrigo, pustular skin diseases. By the age of 6-8, a child's skin is closer to the skin of an adult in terms of structure and function.
In aging, the skin gradually fades: the filling of its blood decreases, weakens the function of the sebaceous and sweat glands, partly they atrophy. Thin skin sometimes resembles cigarette paper and loses its elasticity. The subcutaneous fatty tissue thinns out, disappears completely in some places. On dry, unevenly pigmented skin there are corneal areas - senile ketaromas. It is covered with fine and deep wrinkles, becomes irritable and easily traumatized. Skin regeneration processes worsen, which is associated with the slow healing of wounds. Because of the increased fragility of the walls of blood vessels at the slightest injury and without it there are hemorrhages in the skin.
Age features of the skin in children
Skin features of children. Along with other inherent physiological functions the skin is an organ of protection of an organism from harmful influences of external environment. Skin receptors transmit perceived irritations to the cerebral cortex through the reflex paths. The system of analyzers gradually develops in a child the ability to correctly assess the sensations. This leads to the correct orientation of the child in relation to different types of external influences and develops precautions in relation to harmful influences. Due to the tenderness of the epidermis and the relatively weak development of the connective tissue base - the dermis - the child's skin is easily vulnerable. At the same time, its highly developed vascular system makes the reaction of children to external influences particularly intense. For older children is characterized by the prevalence of diseases with different forms of streptodermia. It should be noted that they have more fungal diseases, in particular candidiasis, than adults. Allergic diseases in children are often influenced by food allergens. Many skin diseases in children (e.g. eczema, neurodermatitis, psoriasis) have a tendency to spread, up to the generalization of the process, and to exudative phenomena. Children are particularly susceptible to viral diseases. They are much more likely than adults to have warts and infectious molluscs. The regenerative capacity of the skin in children is increased. There is a faster epithelialization, faster formation of granules with violations of skin integrity. In various skin diseases in children can easily develop complications associated with weakening of the body's defenses. Acute infectious diseases in children often lead to a deterioration in the course of existing skin disease in the child or the emergence of a new skin.
Skin Hygiene
Skin hygiene is of great importance to prevent not only skin diseases, but also a number of other diseases, especially gastrointestinal diseases. For skin care it is necessary to have special baths for bathing, soft sponge, baby soap, solutions of potassium manganese oxide and boric acid, sterile vaseline or sunflower oil, cotton wool and cotton sticks, gauze swabs, small scissors, etc.
From the age of 2-2.5 children should be taught to wash their hands, wash their hands with any contamination, after playing with sand, animals, after visiting the restroom and especially before eating.
Children should not be wearing wet or moist clothing that will help them to cool down quickly. Diapers and other clothing soaked in urine should not be dried unprocessed, as they become stiff, retain the smell of urine and promote the growth of germs. If the baby is dirty, wash it with warm water (36-37 °), gently applying a soft towel or sheet, and wrap it in clean dry underwear. Every day you should lubricate with petroleum jelly or sunflower oil in those places where it is easy to create diaper. It is not recommended to use powders, as they often cause skin irritation by rolling into lumps.
If the child often regurgitates, to prevent the formation of intertrigo around the neck and behind the ears should be placed between the neck and underwear a small diaper, folded in the form of a napkin, the ends of which are put behind the head.
Hygienic bath should be done for children under two years of age at least twice a week, and in subsequent years, at least once a week with a mandatory daily washing of the genitalia and legs.
Before bathing, clean hands rinse the bath with hot water and soap and pour warm water into it (36-37 ° C). Bathing is conducted at an air temperature of 20 ° C. The child's body is washed with a soft sponge or mitten, specially sewn from a soft cloth. During the bath, make sure that water does not get into the eyes, ears and nose of the child. After washing the body, head and face washed with clean boiled water, and then poured water, whose temperature is 1-2 ° below the temperature of water in the bath.
After bathing, the child's body is gently wiped with a soft sheet, and the skin folds are greased. Clean, wiped with alcohol scissors cut the nails on your fingers and toes. After bathing, rinse and dry thoroughly. Do not wash laundry in it, even children's laundry.
Adults caring for a child, before approaching him, should wash hands, remove rings, pins, brooches and other sharp objects that can hurt his skin. You should examine the body of your child daily. If even a slight redness or rash appears, your child should be examined by a doctor. Minor injuries should be rinsed with water and lubricated with iodine, diamond greenery or "Novikov's liquid".
Reasons for skin diseases
Changes in the condition of the skin in children and the visible mucous membranes may be due to different causes. The younger a child is, the easier it is to develop and, as a rule, more severe skin diseases. This is due to the fact that children's skin is gentle and vulnerable, and the body's resistance to various harmful influences, including microorganisms, is still insignificant. Insufficient regulating influence of the Nervous system, internal secretion glands at an early age often leads to a peculiar flow of skin diseases, and the wealth of children's skin with blood and lymphatic vessels makes the reactions more intense.
Some skin diseases are associated with congenital defects of the skin and manifests itself in the form of improper cornification, bubble formation and other lesions on the skin. Other skin diseases are only symptoms of infectious (measles, scarlet, varicella, rubella) or non-infectious (nervous, endocrine, gastrointestinal) diseases. In such cases, limited or widespread lesions in the form of rashes, eczema, hives, etc. appear on the skin of a child. Some children may have skin lesions due to their poor tolerance of either certain foods or certain odours or medicines. In each case, the cause of the skin lesion must be investigated and eliminated. If a child reacts sensitively to foods that are important to the body or to odours that are common in the environment, it is advisable to train them carefully and gradually.
Skin diseases may also occur as a result of mechanical, chemical and thermal factors as well as radiant energy. Any skin lesions may be complicated by pustular, fungal and other diseases.
In some cases, pustular, fungal, viral skin diseases occur independently. Great mobility of children, their inclination to play with the ground, in the sand, with pets often lead to damage to the skin, resulting in microorganisms easily penetrate through the skin. This happens particularly often in poor hygiene conditions or when children lack the hygiene skills to properly care for their skin. It should be remembered that most pustular, fungal and viral diseases are contagious and can easily be transmitted to a child from sick people and animals.
Changes in the normal condition of the child's skin and visible mucous membranes can inform caregivers about the possibility of certain infectious diseases. In such cases, appropriate measures should be taken to prevent their spread (rubella, measles, scarlet, varicella, pustular and fungal skin lesions, conjunctivitis, etc.). Such changes include the appearance of so-called primary morphological elements of the rash: speckles, spots, nodules, vesicles, blistering, blistering, pustules.
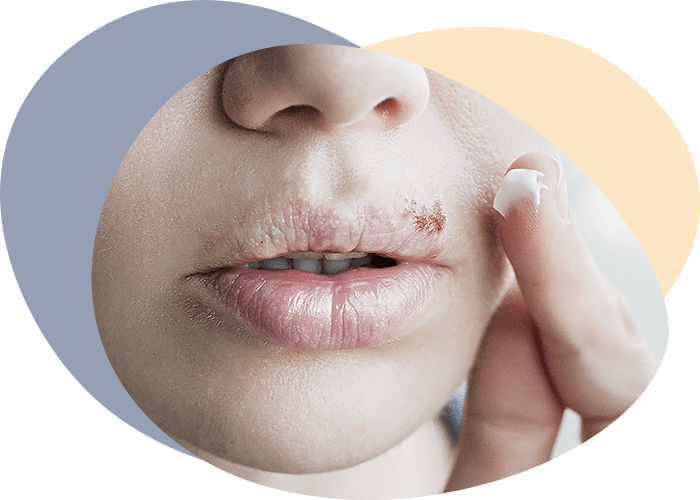
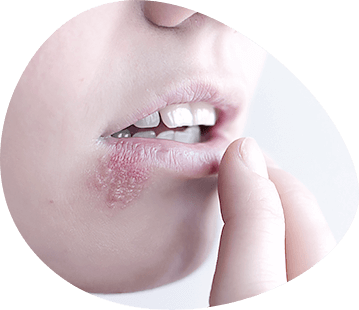
Simple herpes
Herpes simplex is a viral disease caused by the herpes simplex viruses of two HSV-1 and HSV-2 serotypes.
Type 1 herpes simplex virus, whose visible symptoms are called colds, infects the face and mouth and is the most common form of infection. The second most common form of infection is herpes simplex virus type 2, which causes diseases of the genital organs. Herpes simplex viruses are very easily transmitted through direct contact with lesions or with the bodily fluids of an infected patient. Transmission can also occur in skin contacts during periods of asymptomatic disease.
Prevention of herpes simplex
At present, there are no cures or vaccines to prevent infection. However, there are medicines that limit the multiplication of the virus and its transmission through the skin and soothe itching during symptomatic periods of the disease. The main prevention is personal hygiene.
Herpes zoster
Herpes zoster (synonymous with herpes zoster) - a disease that is a reactivation of a sleeping viral infection, which affects the nervous system and skin.
Disease affects people who have previously suffered from varicella. Disease mostly elderly and old people. In contact with previously sick children with a shingles lichen patients they develop a typical varicella.
The causative agent is the chicken pox virus. Outside the acute localization of the virus - the posterior roots of the spinal cord and intervertebral nerve nodes.
Highlight the following clinical forms of the disease:
- gangliocutaneous;
- auricular and ocular;
- gangreneous (necrotic) disease;
- herpes zoster with defeat of vegetative ganglia;
- meningoencephalytic;
- dyseminated (widespread).
Any form of shingles may be accompanied by defeat of the vegetative nodes of the nervous system with the development of unusual for shingles shingles signs (delayed urination, constipation or diarrhea). If the motor branches of the nerves are affected, paralysis may occur.
Preventing shingles
The prevention of this disease can be any form of hardening and increasing the resistance of the body. In old age, when herpes zoster most often affects people, the best prevention is an active motor regime and maximum outdoor stay.
Warts
A warthog is a predominantly benign skin neoplasm, often with a viral etiology that looks like a knot or papilla. It is caused by different viruses of human papillomatosis.
A distinction is made between common, flat, pointed condylomas and senile warts. Ordinary, flat warts and spiky condylomas are caused by a virus common to them. Incubation period is 2-5 months.
Warts prevention
It must be remembered that the warts virus thrives in humid environments. For this reason it is not recommended to walk barefoot in public places such as swimming pools, saunas, baths, use other people's towels, wear tight leatherette shoes. Cuts and small cracks in the hands also contribute to the appearance of warts, which is why you should always treat damaged areas of the skin carefully.
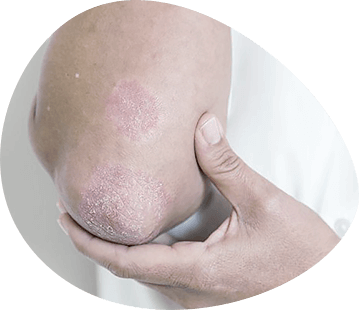
Dermatitis
Dermatitis is a contact island inflammatory lesion of the skin resulting from exposure to irritants of chemical, physical or biological nature. Relates to the group of allergodermatosis. Allergodermatoses - a heterogeneous group of skin diseases, the leading importance in the development of which is attached to an allergic reaction of immediate or delayed type. This group includes allergic dermatitis, toxicodermia, eczema, atopic dermatitis, and hives.
There are 3 different stages:
- Acute (micro vesicular or macro vesicular) - occurs immediately after contact with an irritant and disappears when contact ceases.
- Acute (cortical or flaky).
- Chronic (Acontotic) - occurs in periodic contact with an irritant for a long time.
It is based on allergic reactions of immediate and delayed types. Allergens can be chemicals, medicines and cosmetics.
Allergens are often haptens that form a complete antigen when combined with skin proteins. Macrophages play an important role in forming the manifestations of the disease, as they bind to allergens in the first few hours.
The primary elements are papules, vesicles, oedemas, plaques. Secondary elements are cracks, crusts, flakes.
Symptoms of most dermatitis: inflammatory redness, puffiness, itching, burning, increased skin temperature in the area of inflammation, a feeling of heat in the area of inflammation, the appearance of blisters, bubbles.
The most common forms of dermatitis
Simple contact dermatitis
Appears immediately or shortly after contact with an irritant. The area of impact corresponds to the area of contact. Causes: unconditional irritants (pressure, temperature, acid and alkaline effects, friction, plants). With simple contact dermatitis, the skin tissue is directly affected. Appearance and leaking is determined by the force of action (degree of burn, frostbite). To prevent contact dermatitis, it is necessary to remove the irritant from the skin.
Allergic dermatitis
Called an allergic reaction to some kind of allergen. Like all forms of allergies, it occurs in individuals who are predisposed to this reaction. It is a typical allergic symptom on the skin.
Allergic contact dermatitis
Unlike allergic dermatitis, it does not occur immediately but after contact with an allergen. In order for an allergic reaction (sensitization) to form, it takes between one and several weeks and the body becomes sensitive to the allergen, the next contact will develop dermatitis.
The area of the reaction may exceed the area of contact. The allergen that has come into contact with the skin is captured by the epidermis cells and partially transformed into lymphoma, where it is encountered by the immune cells of the T-lymphocytes, they activate the entire defense mechanism and the skin becomes sensitive to the allergen. Healing inflammation often leaves scabs and scales. Symptoms: bright redness of the skin, bubbles, oedema.
Allergic dermatitis occurs depending on the sensitivity of the body to an allergen and is usually inherited.
Swaddling dermatitis
It is an irritation of the skin of the buttocks and/or inner thighs in infants - young children - caused by physical, chemical and microbial environmental factors. PD is a frequent pathology in children in the first months and years of life, which is explained by the peculiarities of the skin of infants, as well as defects in their care. The prevalence of PD in infants is as high as 50%. It is reported to be more common among girls and prevalent among infants in the second half of life (6-12 months). The main complication of PD is skin infection. Skin changes at PD have no specific (morphological) features. Two products are absolutely indispensable in the care of the skin areas subject to AP: diapers and the so-called "barrier" (protective) cream. The latter is recommended to be applied to the skin "panty zone" at least as often as changing diapers (disposable or regular).
Prevention of diaper dermatitis. The basis of PD prevention is regular and adequate care for the child's skin. There are a number of uncomplicated interventions that should be recommended to avoid the development of PD in the baby:
- not to use baby powder;
- full use of a modern range of baby cosmetics (lotion, cream, oil);
- frequent washing of the child with warm water and baby soap (immediately after each defecation and facial);
- elimination of intense rubbing of diapers, nappies and clothing items in places with natural folds;
- precise selection of diapers by size;
- taking into account the sex of the child when choosing disposable diapers;
- timely changing of diapers. In particular, the change should be carried out early in the morning (immediately after waking up), just before the baby goes to bed, after each meal, if the child shows signs of anxiety;
- use barrier cream every time the baby changes a diaper;
- regular intake of vitamin D. preparations. With rickets, children may experience increased sweating and disturbance of skin structure.
Allergic (atopic) dermatitis or childhood eczema
These skin manifestations are not a skin disease. It's just a skin manifestation of an allergic reaction. Due to immaturity of the immune and digestive systems, lack of detoxifying liver function, some substances entering the body are not absorbed. They cannot be fully digested in the intestines or neutralized by the liver. These substances, as a result of certain conversions, acquire antigen properties and cause antibody production. Antigen-antibody complexes provoke a rash. There are three ways the allergen enters the child's body:
- Food allergies during eating or drinking;
- in direct exposure to the skin, contact allergies;
- respiratory allergy during breathing.
Symptoms of diathesis (allergic dermatitis) are varied - red spots, rashes in the form of red dots, spots and spots, often itching, peeling and dry skin, cracks, ulcers and ulcers.
Prevention of diathesis includes prolonged breastfeeding and adherence to a lactating woman's diet, proper feeding, competent feeding of the child and timely detection of intestinal dysbacteriosis. Allergic dermatitis is usually a temporary phenomenon. As the child grows, liver and intestinal functions and the immune system improve. There is even the term "outgrowth of allergies".
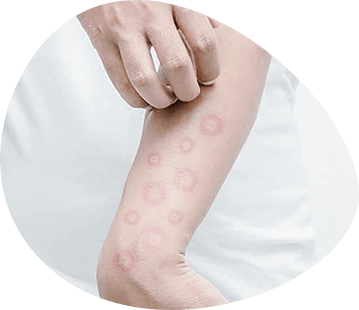
Hives and swelling in Quincke
This is an allergic skin lesion accompanied by vascular wall permeability disorder and swelling of the skin and other organs. Children complain of excruciating local skin itching, chills, nausea, abdominal pain, sometimes vomiting. With swelling Quinque no skin itching, but there may be a feeling of tension, increasing the size of the lips, eyelids, nose, ears, tongue, joint area, as well as difficulty swallowing, stiffness of the voice. Allergic swelling of the larynx, brain, internal organs may occur. In case of occurrence of the above symptoms of the child it is necessary to urgently show the doctor.
For treatment and subsequent prevention of urticaria should be diagnosed and eliminate the allergen that causes it. For example, if an allergy causes a certain type of food, the child should not be given this product. In the acute phase of urticaria children are prescribed desensitizing and antihistamines (tavegil, dimedrol, suprastin).
Usually by the age of 3-7 years, children suffering from urticaria are completely cured of this disease. But chronic urticaria may also be observed as a complication and consequence of other diseases: kidneys, liver, gastrointestinal diseases, worms, chronic tooth infections, gallbladder infection, etc. Then you should treat these very diseases, a symptom of which is hives.
Prevention of dermatitis
Compliance with occupational and domestic safety regulations; timely rehabilitation of focal infection and mycosis of the feet; use of antibiotics and other sensitizing drugs strictly according to indications, taking into account their tolerance in the past.
Articles
Sweatshirt and intertrigo
Sweat and raspberry are non-communicable skin diseases that most often occur with improper childcare.
Sweat - skin irritation caused by the accumulation of a note under the epidermis, can occur in a child with excessive wrapping, rare bathing. When sweating on the skin of the body, in the folds and contact surfaces, the skin of the occiput and scalp usually simultaneously occur multiple pustules the size of a pinhead, are surrounded by a small inflammatory rim. By increasing in size and spreading out over the body, weakened children can become infected with sepsis.
To prevent sweating of the child should bathe regularly, use modern skin care products (highly purified mineral oil, cream, powders, napkins), do not bathe when swaddling, timely change diapers (diapers). Air baths are useful, during which children lie naked in a warm room, and in summer - in the air in the shade.
Defactness - redness, sloughing of the skin, the appearance of cracks in its folds. Occurs in children in cases where they do not change long wet clothes, diapers, rarely bathe them. Most often oprelost appears in the inguinal folds, armpit pits, neck, behind the ears. Touching the skin in places of intertrigo is very painful. The child becomes restless, capricious, sleep and appetite are disturbed. Baby skin in these cases, it is recommended to treat with baby cream, which, having a bactericidal effect on microflora, prevents the formation of excessive moisture and natural excreta. You can also use modern powders that effectively reduce skin friction inside the skin folds and about the tissue. The powder should not be applied directly to the child's body, and with the help of the palm should be evenly distributed in places of formation of interleavage.
With frequent regurgitation to prevent the formation of intertrigo on the neck and behind the ears between the child's neck and underwear lay a small special tissue, the ends of which are placed behind the head. The regurgitated masses will not fall on the child's skin, underwear and pillow. After each regurgitation napkin must be changed.
Bathe the child in the presence of interleavage need boiled water or a weak solution of potassium permanganate. After bathing the body and skin folds drained with a soft sheet, places of interleavage treated with cream or powder. Service personnel of the children's institution should carefully inspect the body every day, pay attention to the appearance of even small redness, which may later turn into intertrigo. If the child's diaper rash is extensive or untreated, it should be examined by a doctor.
If the skin is dry and "crusts" are formed on it, it is recommended to wipe such places with oil, which moisturizes the skin, is well absorbed and does not prevent the natural breathing of the skin.
Eel
Acne, eels - sebaceous gland inflammation.
The causes of the disease remain unexplained. The main role in the development mechanism is assigned to seborrhea, which reduces the bactericidal effect of sebum and leads to the activation of coccal flora.
Common acne (juvenile eels, acne disease) develops in boys and girls during puberty and gradually disappears by 25-30 years. The appearance and exacerbation of acne is also affected by menstruation, stress, fever, high humidity and genetic factors. Acne is also known to be caused by cosmetic products containing lanolin and paraffin. Acne may also be a side effect of some medications.
Seborrhea, hyperplasia of sebaceous glands, hyper-secretion of sebum, hyperkeratosis leading to the formation of comedones - sebaceous corneal plugs in the ducts of sebaceous glands with partial or complete clogging, which look like black spots, are pathomorphologically noted.
Acne is an inflammatory disease of the skin caused by changes in the pilosebatic structures (consisting of the hair follicle and sebaceous gland).
Among the causes it is distinguished:
- heredity
- hormonal activity (menstruation, puberty)
- awkward age
- adrenal stress
- overactive sebaceous glands
- dead skin cell accumulation
- microorganisms
- inflammatory skin lesions
- anabolic steroid use
- use of preparations containing halogens (chlorine, bromine, iodine), lithium and barbiturates
- exposure to high doses of chlorine (e.g. occupational hazard)
Preventing eels, acne, acne
Prevention of acne (acne, acne) is a healthy way of life, strengthening immunity, the exclusion of the above causes of acne. To prevent exacerbation of acne should be excluded from the diet: chocolate, oil, fat, spicy food, alcohol.
Many patients suffering from acne noted improvement in the summertime. Ultraviolet has a disinfectant and masking ability. But this temporary effect is fraught with further exacerbation of the disease, as high doses weaken local immune protection, increase salivation and make it even more difficult to reject the skin scales in the sebaceous glands ducts, thereby causing an increase in acne.
Therefore, sunbathing should be done in doses using photoprotective sunscreen and avoiding exposure to the open sun from noon to 4 pm.
Mycoses
A number of skin diseases occur as a result of microorganisms called fungi entering the skin. These pathogens parasitize on the skin of people and some animals, often also affecting hair and nails. Fungal diseases are transmitted from a sick animal or human being, as well as through objects used by patients: hats, gloves, underwear, toys, books, combs, scissors, hair clippers, etc. Scratches, wounds, cracks and other skin damage contribute to the infection. Healthy skin prevents fungi from penetrating deeper layers of the skin. There are several types of fungal diseases.
Mycoses - (fungal diseases), human and animal diseases caused by microscopic pathogens (fungi).
Mycoses are divided into 4 groups. Keratomycosis (branched lichen, erythrazma, nodular trichosporia, or piedra, armpit trichomycosis) - poorly contagious diseases. Their agents parasitize in the most superficial parts of the corneal layer of the skin (inflammatory reaction is not caused), as well as on the cuticle of the hair, without affecting its substance. Epidermomycosis (epidermophytosis of inguinal and foot, rubrophytosis and superficial yeast lesions - candidamycosis) are contagious and very common among the population of all continents. Pathogens parasitize in the stratum corneum, often affecting the nails, accompanied by a pronounced inflammatory reaction. Trichomycosis (trichophytosis, microsporia and scabies) - the most infectious dermatomycosis with serious social and hygienic significance. Affect smooth skin, hair and nails. In most cases, the mushrooms located inside the hair and affecting its substance, cause superficial skin lesions, and mushrooms that parasitize around the hair, causing deep damage. Deep dermatomycosis - actinomycosis (according to modern concepts, actinomycetes belong to mycobacteria), deep blastomycosis, chromomycosis, sporotrichosis, coccoidomycosis, histoplasmosis, as well as mycosis caused by some mold fungi. Their pathogens parasitize in deep layers of skin and subcutaneous tissue, penetrate into internal organs, muscles, bones, lymph nodes, causing their lesions. The skin usually produces large nodular or tumor-like sprawl, disintegrating or necrotizing, turning into ulcers, slowly healing with the formation of deforming scars.
Trichophytosis - (from buckwheat hair, phyton plant) in everyday life is called ringworm.
The source of the disease is a sick person or things that he used. Some types of disease are transmitted from animals (horse, cattle, dog). Children are mainly affected, most often boys aged 4 to 15 years. The incubation period of the disease ranges from a few days to 1.5 months. Smooth skin, scalp and nails may also be affected by the disease. On the skin, most often on the face, neck and hands, sharply limited itchy pinkish-red round spots are formed. They have a tendency to spread, can merge with each other and are further flaked. Both skin and hair are affected on the head. The mushrooms are introduced into the hair bags, and from there into the hair, which lose their shine, become matte, as if dusty, easily broken. The skin of the affected scalp is covered with grayish-white scales. When the affected nails in the thicker they are formed grayish or yellowish spots. The nails lose their shine, become brittle and their edges easily crumble. In a microscopic examination of the affected skin, hair and nails found in them colonies of mushrooms. Timely and proper treatment contributes to the favorable outcome of the disease, and hair growth in the affected areas is restored.
Types:
- Trichophytosis is superficial.
- Trichophytosis chronic.
- The trichophytosis is infiltrative-negative.
Scabies - a disease that occurs as a result of penetration under the upper layer of the skin of the hands, feet, and sometimes the torso of scabies. Itchy tick belongs to the arthropod family. In 95% of cases, infection occurs through prolonged and close contact with a sick person. Indirect transmission is possible through clothing and bedding. The natural resilience of the tick extracted from human skin is quite weak: adult forms live no longer than 2 days at 22 ° C. At temperatures above 55 ° C, the tick dies within 10 minutes.
Thermal treatment of things (washing laundry and bedding at water temperatures above 55 ° C) practically eliminates the possibility of indirect transmission of the pathogen.
An adult fertilized female tick, getting to the surface of the skin, within about an hour drills the horny layer of the epidermis with claws at the ends of its front legs, making vertical holes. It then digs S-shaped scabies parallel to the skin surface. The female progresses in the scabies at a rate of up to 5 mm per day. A few hours after the scabies are formed, she begins laying 2-3 eggs a day. 3-4 days after laying the eggs, larvae are formed from them, which leave the scabiest course, drill the skin and come out to its surface and return to the epidermal layer of skin. Bites of the larvae cause itching and combing, in which often the skin gets a secondary infection, most often purulent. Favorite spots of scabies - hands, areas with the thinnest, most delicate skin between fingers, on the bends of the joints, the bottom of the abdomen. The parasite never affects the skin of the face and the scalp. The whole cycle of development of a mature tick occurs in about 10-14 days. Life expectancy of the parasite can reach 2 months.
Scabies should be immediately isolated from others. The patient's body and bedding are boiled, and blankets, mattresses, pillows and top dress are chemically disinfected or ventilated for 10-12 days. Over-affected children are admitted to the team only after a complete cure.
Prevention of mycoses
In infectious surface mycoses - timely isolation and treatment of patients, removal of the source of infection. Quarantine is established in children's institutions, which is cancelled 4 weeks after the last case of trichophytosis, favaus or microsporia, and 6 weeks after the last case of microsporia. If there is one child in the family who is ill and the treatment is carried out on an outpatient basis, other children are not allowed into the children's group during this period.
The basis for the prevention of superficial mycoses, and especially foot mycoses, is strict observance of the rules of personal hygiene and the sanitary and epidemiological regime in baths, swimming pools, showers and hairdressers.
Prevention of deep mycoses lies in the timely treatment of wounds, abrasions, the use of respirators when working in dusty rooms, on earthworks.
Pustular diseases
Children's skin is easily polluted, while playing or working on the site, in the garden or vegetable garden. Dust, dirt and microorganisms contained in them - staphylococcus and streptococci - are embedded in the skin grooves, hollows and irregularities. The mud irritates the skin, causes itching and combing, through which, as well as through scratches, abrasions and wounds, heterogeneous microorganisms penetrate deep into the skin, often causing pustular diseases. The less skin is damaged and contaminated, the less pustular diseases occur. The weaker the child, the less resistant his or her body, the more susceptible his or her skin is to the harmful effects of microorganisms. Pustular diseases are therefore particularly frequent during or after various diseases. Excudative diathesis, diabetes, anemia, gastrointestinal diseases, as well as fever, hypothermia, tight, uncomfortable and especially dirty clothes contribute to the emergence of pustular skin lesions. Getting a drop of pus from the patient's pustule on the skin of a healthy child can cause a similar disease. Among the various skin diseases in children, pyodermia is about 40%. Pustular diseases most often occur in the form of streptodermia and staphylodermia.
Streptodermia is a pustular skin lesion caused by streptococci; it is characterized by superficial lesions of smooth skin and its folds (impetigo, seizing, paronichia).
Impetrigo (from Latin - sudden) is characterized by high contagion and is characterized by bubble rash on a reddened background. At the place of penetration of a homogeneous microorganism, more often on the open parts of the body; corners of the mouth (zaeda), behind the ears, the roller of the nail (paronichia) - first a red spot or swelling is formed, and then a vial the size of a pin head to ten kopecks. Soon the vial turns into a pustule, which when dried is docked thin orange-yellow crust ("honey crust"). Next to form new bubbles and crust. The disease easily passes not only from one place of the skin to another, but also from one child to another, so the patient should be separated from other children. Towel, dishes, napkins of the patient are stored separately. Toys and things that he used to wash with hot water and soap, and even better to boil. The patient is treated only as prescribed by the doctor.
Staphylodermia - pustular diseases caused by staphylococcus; characterized by lesions of skin appendages (hair follicles, sweat and sebaceous glands).
Folliculitis - inflammatory lesion of the hair pouch. The disease is characterized by the appearance of small, 1 -2 mm pustules, permeated in the center of the hair and surrounded by a narrow pink border. In a favorable flow after 3-4 days, the contents of pustules dries up, yellowish crusts are formed, after the fall off which leaves no traces on the skin.
Furuncles (tweezers) - acute inflammation of the hair follicle, sebaceous gland and subcutaneous fatty tissue. Within 3-5 days, the boil increases, reaching the size of a hazelnut and more. The skin in the area of the boil turns red, thinning. After autopsy, dead tissue and ulcer can be seen in the centre, and after healing the scar remains. If necessary measures are taken in the early stages of development of the boil (application of a clean ichthyol bandage, physiotherapy, etc.), it may dissolve and the scar will not form.
Carbuncle - the suppuration of several follicles located nearby. Large areas of subcutaneous adipose tissue are inflamed. There is an ailment, headaches, increased body temperature. The disease sometimes lasts more than a month. It is especially dangerous if carbuncle is formed on the face, as the purulent process can penetrate the brain membranes.
Prophylaxis
In the case of pustular diseases should not be used compresses, as, softening the skin, they contribute to the spread of purulent lesions, for the same reasons should not take baths and showers. Undamaged skin should be wiped daily with alcohol in half with water or vodka, short cut nails, nail spaces lubricate with antiseptic solutions. All this protects healthy body parts from infection with pustular infection. In case of pustular diseases it is not recommended to give children chocolate, honey, jam, sweets, spicy foods and smoked foods. To prevent pustular diseases it is necessary to increase the overall resistance of the body, to provide a complete diet with sufficient vitamins, the right mode, to comply with hygienic rules of skin and clothing care.
Hydradenite - a purulent inflammation of apocrine sweat glands, which do not occur in children.
Conclusion
So, skin is the natural cover of the berrier between the body and the environment. Skin performs the function of protecting the body from adverse effects.
Skin disease should always be considered a general disease of the whole body. But in turn, skin diseases can have a sharp and deep impact on the whole body.
The condition for maintaining a healthy skin is to keep it clean, rules of personal hygiene, active exercise, stay in the fresh air, proper nutrition.
It is also important to remember that, as with any disease, skin diseases are easier and better to prevent and prevent than to treat them later. It is always easier to maintain what is given to us by nature in a normal way than to restore it later.