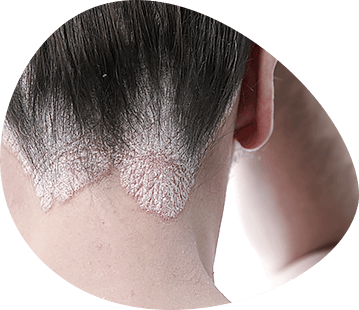
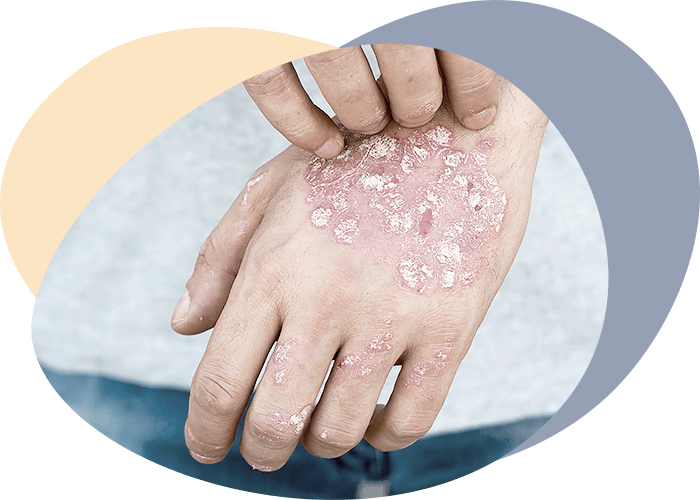
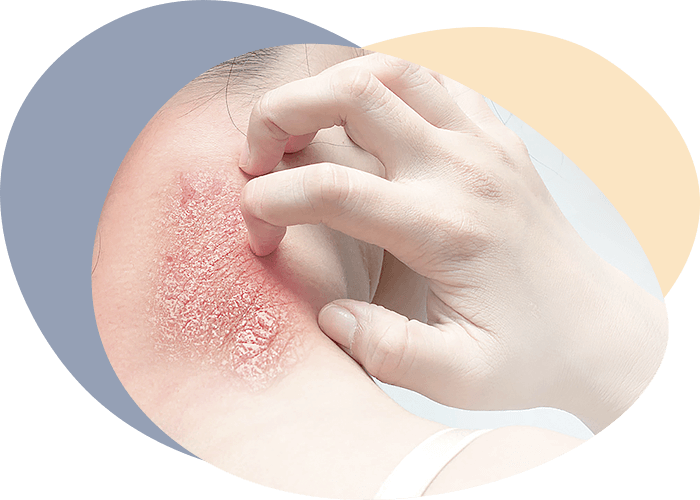
Clinical characteristics of psoriasis
Psoriatic skin efflorescences are often characterized as monomorphic due to the fact that the recognized primary element is papula. However, in psoriatic erythrodermia, the primary element of erythema can be seen, and in patients with pustular psoriasis - pustule. In addition, a spotted type of psoriasis is described. Therefore, diagnosis of psoriasis is difficult, requires a diagnostic biopsy.
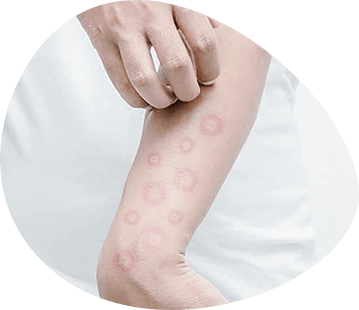
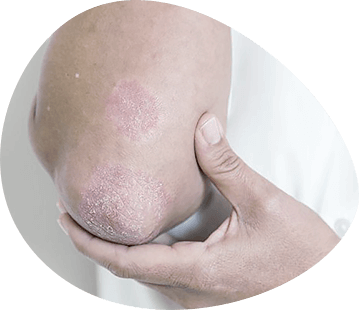
During psoriasis there are three stages: progressive, stationary and regressive. At the stage of progression of the disease papules color is brighter, they are swollen, tense. Around the papules is defined a clear spotty erythematous edematous border (peripheral pink growth corolla). Many papules are in a state of fusion, merging into large areas of papule infiltration or plaques of different shapes. The progressive stage of psoriasis is characterized by a positive Cobner enzyme. It is manifested by the formation of papuletic elements at the friction and pressure points. Usually in these cases, papules are located linearly, repeating its localization of the irritation. The Kobner phenomenon is explained by the presence of such a pronounced hyperergic state, in which even apparently healthy skin is in a state of readiness for inflammatory response. The slightest, even physiologically normal tension or pressure (e.g. the area of the waistband or bra strap, sometimes in place of a scratch or comb) is accompanied by the formation of a papulegic rash. In the stationary stage, the peripheral growth of the sprinkling elements stops, the papules flatten and turn pale. The formation of ring-shaped hearths is possible due to intensive resolution of infiltration in the center. Sometimes papules and areas of papuloid infiltration are resolved from the periphery rather than the center. Then papuletic elements seem to melt from the edges and lose their properly rounded shape. Period of regression is characterized by the complete disappearance of papuletic infiltration on a large surface of the body with the formation of former rashes in place of hyperpigmentation centers or areas of secondary "false" leukoderma. Around the regressive psoriatic elements one can often see a pale, as if folded edging - D.L. Voronov's pseudoatrophic bezel - a symptom of active process resolution. In addition to the typical, classical form of psoriasis psoriasis is distinguished by atypical varieties:
- exudative;
- spotted;
- seborrheic;
- old-timers;
- bearded psoriasis;
- irritated;
- intrigenous.
Exudative psoriasis. This variety is often observed in persons overweight, with diabetes or with reduced thyroid function (stat. mixedematicus). The process is manifested by foci of acute edematous inflammation with not sharply pronounced and sometimes absent infiltration, with vague, irregular outlines, with abundant layering uncharacteristic for psoriasis of serous or serous-purulent crusts and cortical-shell. Quite often, patients with exudative manifestations of psoriasis have wetness, intense itching, which complicates diagnosis, the localization of exudative psoriasis is unique: more often the centers are located on the lower limbs or in large skin folds.
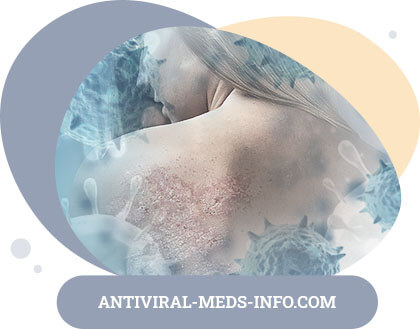
Spotted psoriasis (psoriasis). This form is distinguished by the presence of erythematous spots, sometimes with little or no infiltration, but with abundant characteristic peeling and the presence of pathognomonic psoriasis triad. It should be noted that spotted forms of dermatosis are observed mainly in young women, so it is called "female" psoriasis.
Seborrheica psoriasis. This species is the most difficult to diagnose, because it includes in clinical symptomatology features of the clinic of seborrheic eczema and manifestations of seborrheic status in patients. As a rule, in seborrheic areas (the hair part of the head, nasolabial and nasolabial folds, behind the auricles, on the chest and in the intertropatular region), seborrheic elements with abundant coarse-plate peeling are detected. Foci on the face and chest of the bowl are represented by spotty rashes with oily grayish-yellow scales imitating seborrheic eczema. Behind the auricles you can see areas of infiltration of deep pink or red also with abundant gray or gray-purple crusts, with the presence of cracks, wetness, simulating a picture of streptodermia or seborrheic eczema, complicated by pyodermia. However, papuletic infiltration elements are always found on the scalp, and on the forehead skin on the border with the hair psoriasis patients usually have papules with characteristic peeling. They are either sporadic, separately located, or pass from the scalp to the forehead skin in the form of a crown ("psoriasis crown").
3-year-old psoriasis (pSor. inveterata). This variety is manifested by the long existing papule drainage areas, with sharply pronounced infiltration, with clearly delineated boundaries. Due to the presence of a powerful inflammatory infiltration, long current, the color of the centers acquires a brownish tint, the surface of the papules is hypertrophied with the formation of hyperkeratosis and warped sprouts (pSor. verrucosa).
Irritated psoriasis (pSor. irritabilis). Sometimes due to irrational treatment, excessive insolation, stressful situation in the life of patients there is a rapid increase in inflammatory response. Papulegic efflorescences become swollen, acquire an intense, bright, saturated red color. Around the papules quickly appears swollen hyperemic belt, which promotes the fusion of individual rashes in a continuous diffuse lesion of large areas of the skin, often turning into erythrodermy. In case of irritated psoriasis, as well as in the progressive stage, reactivity with polyvalent hypersensitivity phenomena increases significantly. As a result, new fresh papulegic efflorescences (the Kobner phenomenon) appear even on healthy skin areas with minor irritation (friction, pressure, scratch).
Intertriginosa psoriasis. The location of psoriatic elements in large skin folds is an atypical localization and is typical for untidy patients with diabetes, obesity, and vegetative dystonia. In this form of psoriasis in the armpit cavities, interannual, inguinal and interfinger folds, under the mammary glands there are oedematous, erythematous-papulegic foci, often wet, erosive with detached corneal layer on the periphery. Intrigenous psoriasis may resemble candidiasis, rubromycosis, epidermophytosis. In contrast to psoriasis, candidiasis and dermatomycosis of large and small folds are sharper, the surface of the lesion centers is brighter. The edge of the affected areas is clearly marked by a kerb of the "undermined" stratum corneum. On the periphery, as a rule, elimination in the form of spotty and vesicular efflorescences can be seen.
In addition to atypical clinical forms of psoriasis, there are severe varieties that require special attention in terms of diagnosis and treatment. These include:
- psoriatic erythrodermia,
- pustular psoriasis,
- arthropathic psoriasis of the nails
- psoriasis of the mucous membranes.
Psoriatic erythrodermia. The direct factors contributing to the formation of psoriatic erythroderma are various provoking moments. We had to observe the development of erythroderma after angina, nervous-mental, traumatic effects, after irrational use of UVA, sun exposure, taking antibiotics, sulfonamide preparations, methotrexate, use of irritating ointments. In these cases, separately located efflorescences are activated, acquiring swelling, bright saturated erythematous coloring, forming multiple figures of the fusion, and in some places - continuous diffuse areas. The papules and plaques become indistinguishable. The skin of the body and extremities takes the form of a dense intense shell, stagnant brown color, intense infiltration, abundantly flaked. Another way of forming psoriatic erythrodermy, the so-called spontaneous idiopathic psoriatic erythrodermy, is possible. Without previous irritation or the action of obvious stress factors rapid development of diffuse stagnation of the skin of the torso and limbs with significant swelling, tension, abundant peeling. The presence of individual typical psoriatic papules on the periphery helps correct diagnostics. Unlike skin lymphoma of the erythrodermic type, psoriatic erythrodermia is not accompanied by pathological hematological symptoms, in histological preparations there are no Sisari cells and accumulation of pathological lymphocytic elements.
Nail psoriasis. Affection of the nail plates in patients with psoriasis always takes place, but the clinical changes are expressed differently. It is common to distinguish two forms of nail pathology: pinpoint and diffuse. In case of dotty lesion in the nail plates are formed dotty, with poppy seeds of different depths. Externally, the nail plates in this case resemble a thimble surface, and psoriasis is called thimble-shaped. Diffuse change of nail plates has different degrees of clinical pathology and is characterized by significant polymorphism. Minimal changes, which are stated in almost any psoriasis patient, are represented by a slight blurring of the surface plate (1amina), grayish shade of color of the nail plate and a subtle longitudinal exhaustion. In case of significant changes of diffuse nail plates, atrophic shape, hypertrophic and psoriatic onychia in the form of footstep hemorrhages are distinguished.
Atrophic onycholysis, or psoriatic onycholysis, is characterized by thinning of the nail substance without previous inflammatory changes, the nail plate, gradually thinning, is separated from the nail bed or, gradually licked, disappears, up to the remains of the nail plate grayish in the hole. Thinning of the nail plate and its licking often begins at the free edge of the nail, but it can also occur on its side areas.
The clinical variety of onychodystrophy of hypertrophic type is manifested by various changes in both shape, color and consistency. Thickening of the nail plate with deformation and change of color from grayish-yellow to dirty-gray occurs most often. The nail plate loses its luster and becomes dull, uneven, bumpy. Deformation of the nail plate begins with the manifestation in the region of the hole bore Bo. Infiltration increases as the nail plate and the nail bed become involved, and the nail plate thickens and deforms even more. The nail becomes dense, reminiscent of the claw of a bird of prey. This process is called oncogriphosis and more often develops in the foot area. In other cases, the nail plate is destroyed. The nail becomes loose, crumbly, brittle and is gradually rejected, leaving only small loose horn layers at the well.
The psoriatic onychia of the type of nail hemorrhages first described A. A. M. Arievich (1964), who observed two types of hemorrhages. Hemorrhagic spots of the first type, which pass through the nail plate, can be in the region of the well. They are formed by the enlarged capillaries of the nail bed papillae and disappear under pressure. The second type of nail hemorrhages is characterized by spot or striped hemorrhages, which acquire hemorrhagic yellowish-brown or black color, sometimes thin arrow-shaped stripes in the distal part of the nail plate give the impression of a splinter. All lesions of the nail plate are accompanied by swelling, infiltration, stagnation and hypermissible lesion of the pericarpendicular roll (ragona psoriatica). The posterior nail skin is infiltrated, with abundant characteristic peeling, which is absent in onychomycosis and candidiasis. Psoriatic paroniasis is often accompanied by serous, sometimes purulent separation from under the posterior nail roll, which is also the most important differential-diagnostic sign to distinguish psoriasis from candidiasis and mycotic lesions.
Pustulosa. The disease is manifested by surface purulent elements such as streptostafilococcal impetigo... Is distinguished by primary, or idiopathic, pustular psoriasis, which is severe with malignant flow, and secondary benign. The idiopathic variety of pustular psoriasis is characterized by the presence of primary purulent elements, located on an infiltrative base with intensive peeling and the main pathogenetic phenomena typical for psoriasis. In the benign form of pustules usually appear on 6 dummies of vulgar psoriasis or purulent efflorescences replace previously appeared papules. This flow variant is usually called psoriasis with pustularization. It is a persistent current type of psoriasis, often resulting in disability or death. Pustular forms of psoriasis are rare. The main factors of the pustular form of psoriasis are: methotrexate, treatment with corticosteroid hormones, alcohol abuse.
Arthropathic psoriasis (psoriatic arthropatica). Despite significant progress in the study of psoriasis, the most severe and less manageable form of psoriasis treatment in psoriasis patients is arthropathic arthritis. According to a well-established tradition, psoriasis still refers to skin diseases, although it has been established that psoriasis is systemic and can affect not only the skin but also internal organs, nervous system and joints.
Psoriatic arthritis is characterized as a systemic process, in which the most pronounced changes are manifested in the structure of connective tissue. Psoriatic arthropathy can proceed benignly on the type of mono- or oligoarthritis or polyarthritis, and in some patients becomes a severe destructive polyarthritis. Psoriatic arthritis more often occurs in parallel with skin lesions or later, and in some cases, joint syndrome may precede skin efflorescence. Lesions of the joints usually begin in the distal interphalangeal joints of the hands and feet. Gradually, middle and large joints, including the spine, are involved with the development of ankylosing spondyloarthritis. The variety of clinical variants of psoriatic arthropathy and difficulties in its diagnosis have contributed to the creation of a number of classifications, built primarily on clinical-anatomical and radiological criteria.
In clinical conditions, in addition to X-ray and anatomical criteria, it is necessary to take into account the degree of activity and functional ability of bone and joint joints.
For clinicians, the degree of functional failure of the joints is also of significant importance, which is determined by the performance criteria.
The presence of multiple viscero-pathies, in addition to vegetetodistonic and neuroendocrine disorders, makes psoriatic arthropathy especially topical. The progressing asthenic state up to cachexia, myalgia, atrophy of muscles of the hands, forearms, tibia (12 - 15%) attracts attention. As with conventional psoriasis, psoriatic arthropathy patients are determined by the insufficiency of liver and kidney function, immunodeficiency conditions, cardiovascular pathology. It is recognized that lesions of the musculoskeletal system and internal organs in psoriatic arthropathy have no characteristic pathogenetic symptoms and signs, so the diagnosis is based on a comprehensive examination of patients, taking into account the analysis of clinical features of the lesions of the joints, skin and its appendages.
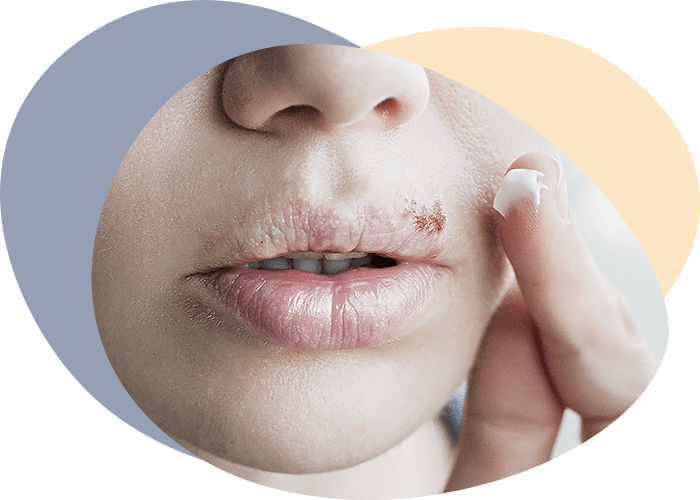
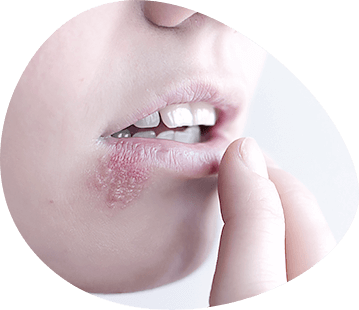
Psoriasis of the mucous membranes. Numerous studies of the pathogenesis of psoriasis have deepened the understanding of the diversity of complex pathology, indicating a systematic process. This was the reason to talk about psoriasis as a psoriatic disease. Affection of the mucous membranes, and in particular the oral mucous membrane, is now recognized. The appearance of psoriatic efflorescences is known not only in the oral cavity, but also on the conjunctiva, on the mucous membranes of the genital organs. Excrescences on mucous membranes often constitute a continuation of psoriatic efflorescences on the skin. Psoriasis of the mucous membranes, as well as psoriasis of the skin, may have varieties. More often psoriasis of the skin and mucous membranes runs synchronously, starts and regresses simultaneously. The most common localization in patients with vulgar psoriasis is lesions of the mucous membrane of the cheeks, red edging of the lips and tongue. The presence of inflammatory elements of rounded, oval or irregular shape, slightly protruding over the surrounding mucous membrane is characteristic. The boundaries of the efflorescence are clear, often sharply limited. The rash is of a drainy nature. There is always a pink edematous border around such a hearth. On the surface of the hearths may be the formation of loose whitish-gray plaque, but more often observed erythematous inflamed surface, slightly oedematous with minor exfoliation of the epithelium by the type of peeling. In patients with widespread psoriasis in the progressive stage or exudative type of the disease, and more often in patients with psoriatic erythrodermia is observed lesion of the lip red border. The process is characterized by an inflammatory zone in the form of a ribbon going from one corner of the mouth to another. The red border is puffy, hyperemic, often infiltrated, with transversely arranged cracks and fine scales and crusts. The most pronounced is puffiness and hyperemia in the Klein zone (along the lip closure line). The process may be localized on one, often lower lip, but may also be on both lips. Psoriatic rashes on the oral mucous membrane are sometimes accompanied by burning, but more often without subjective sensations. In the genital area, psoriatic rashes are more often formed in men on the inner foreskin, and in women - in the transition folds of large and small lips. In contrast to lesions on the oral mucous membrane, this localization clearly identifies the characteristic symptoms of the psoriatic process. Pink, rounded papules with clear borders, prone to fusion and with a layering of grayish-white scales or scales-crown, easily detachable by scraping, are usually visible.
The lesions of the mucous membranes in patients with pustular psoriasis are permanent. Affection of the oral mucous membrane is an essential sign of pustular psoriasis. In accordance with the peculiarity of the skin rash, manifestations of psoriatic pustular efflorescences on the mucous membranes are characterized by the severity of swelling, the presence of serous and purulent exudation, frequent formation of erosive and ulcerative elements.
The differential diagnosis with red flattened psoriasis is based on the characteristic pink coloration of the rash in psoriasis patients with the formation of spot bleeding when removing whitish-gray patina or exfoliating epithelium. Psoriasis differs from leukoplakia by absence of dense infiltration, presence of alternating periods of regress and recurrence of rashes, and also detection of spot bleeding at light scraping. Such factor as synchrony of appearance and flow of rashes on skin and mucous membranes is important for differential diagnostics.
Articles
Treatment of psoriasis patients
Drugs used for general therapy. For the treatment of psoriatic disease, so many different drugs are used that act on multifactorial pathogenetic mechanisms of dermatosis formation that such treatments should be called directed polypragmatism.
Used means of general impact on the body, its internal environment (homeostasis), nerve-endocrine and immunological mechanisms in each case act pathogenetically. However, according to the results of treatment it is not possible to make any conclusions about the cause of psoriasis. Methods of pathogenetic therapy are diverse, so before starting treatment the patient is carefully examined. The examination includes a detailed anamnesis, study of the patient's general condition, its internal organs, nervous and endocrine system, study of the level of activity of humoral and cellular factors of immunity, identification of foci of local infection. The treatment is prescribed taking into account the stage of the disease, seasonality, clinical type of dermatosis (disseminated, limited, psoriatic erythrodermia, psoriatic arthritis, etc.). In the process of selecting pharmacological products specify the drug tolerance, the efficacy of previous therapy, the duration of remission and the cause of the relapse. It is known that a more favorable and quick result of the therapeutic measures is observed with short, uncomplicated, limited types of psoriasis. At the same time, it should be noted that during this period and psychologically ill people tend to trust the doctor more and not to get carried away with self-treatment, which often counteracts the prescription.
Heavy varieties of dermatosis are more difficult and torpid. Much slower comes the remission of exudative pustule, erythrodermic and arthropathic forms of psoriasis. The timely commencement of treatment, combined with a rational regime, with the use of physical, balneo and spa treatment, guarantees long-term clinical remission. Before choosing one or another method of psoriasis treatment, it is necessary to determine the system of the patient's daily routine. If the patient's process is widespread and progressive, it is more appropriate to conduct treatment in hospital conditions.
General treatment of patients with widespread, progressive psoriasis has long been recommended for calcium preparations providing anti-inflammatory, hyposensitizing effect, tightening cell membrane, normalizing adenylate cyclase activity and reducing permeability of derma capillaries. More effective parenteral administration of 10% calcium gluconate solution intramuscular or intravenous 10 ml per day - two 10 - 15 injections per course.
Widely used and other calcium salts - calcium chloride, glycerophosphate, pantothenate, lactate, which have sedative, anti-inflammatory, thickening the vascular wall, as well as reducing the severity of vegetetodystonia. The application of calcium salts in exudative psoriasis is especially shown. Contraindications for their prescription is hypercalcemia, hypertension, thrombophlebitis and symptoms of hypercoagulation, no complications are observed if the drugs are administered taking into account contraindications, desensitizing and anti-inflammatory effects of a wide range is also characteristic of sodium thiosulphate, which is most effective for intravenous administration. It is prescribed as 30% solution in 5 - 7 - 10 ml per day for 20 - 30 days. It is also possible to use 1 - 2 g orally in powders, tablets or as 10% solution in 1 - 2 tablespoons 3 - 4 times a day.
The active anti-inflammatory hyposensitizing agents also include salicylates (sodium salicylate, acetylsalicylic acid), which have cortisone-like effect, as they have a stimulating effect on the synthesis of cortimosteroid hormones. Sodium salicylate is used orally in tablets of 0.5 - 1 g per reception 2 - 3 times a day or as a 5 - 10% solution to 1 tablespoon after meals. When taking sodium salicylate may have side effects: hearing loss, sweating, allergic reactions. To avoid dyspeptic effects, it is prescribed only after meals. Contraindications for the use of sodium salicylate are: gastric and duodenal ulcer, gastrointestinal bleeding, blood clotting disorders.
Antihistamines are not considered to be the main drugs; psoriasis patients are prescribed only when itchy or when psoriasis is acute with hyperergic symptoms. The most commonly used are dimedrol, diprazine (pipolyphen), suprastin, diazolin, tavegil, fenkarol. In addition to histaminolytic action, these products eliminate increased vascular permeability, reduce inflammatory potential of tissues in the reaction of the antigen - antibody. Their hyposensitizing effect is based on neutralizing histamine, serotonin, bradykinin and acetylcholine. These drugs, having the ability to reduce the excitement of the CNS, facilitate sleep onset.
The duration of antihistamine use is limited, as there are three periods in the action of antihistamine drugs. In the first period, there is a pronounced antihistamine action, in the second - there are the phenomena of addiction, usually formed after 1 - 1.5 months and characterized by the loss of therapeutic effect. In the third period, the antihistamine drug itself becomes an allergen and may cause general and local allergic reactions. Therefore, any of these drugs are used in short courses of 7 - 10 - 15 days, but no more than 20 - 30 days. In the treatment of chronic relapsing psoriasis drugs are necessarily changed. More effectively combined use of antihistamines with calcium compounds.
Novocaine and aminazine also have antiserotonin action, which, being synergistic antihistamines, improve their therapeutic effect. In an organism novokoin rather quickly hydrolyses, forming steam-aminobenzoic acid and diethylaminoethanol taking part in synthesis of the folic acid which exchange is broken at psoriasis. Novocaine is injected in various ways: intravenously, subcutaneously, intramuscularly and electrophoretically. For oral administration it is prescribed 1 - 3%, a solution of 1 tablespoon 3 times a day after meals for 3 - 4 weeks. Intramuscular and subcutaneous novocaine is used on different schemes and in different doses. More often 2 % solution is used, injected with 1 - 2 ml daily or after a day for 1 - 1.5 months. Then a break of 1 - 1.5 months follows and the treatment course is repeated. Intravenous injections of 0.25% of the solution of novocaine are made daily or after a day, starting with 2 ml and gradually increasing the dose to 7 - 8 - 10 ml. The course of treatment is 10 - 15 - 20 injections. For better tolerability of novocaine it is recommended to add in one syringe 5 - 7 ml of 25% magnesium sulfate solution. Before starting to administer novocaine in all methods of its administration, it is necessary to determine its tolerability, because hypersensitivity or even intolerance is possible. Novocaine is prescribed at any clinical form and stage of psoriasis, but especially novocaine is indicated in the progressive course of dermatosis.
Aminasin refers to antihistamine drugs, but also has hypotensive, anti-inflammatory and sedative effects. It reduces capillary permeability and reduces the inflammatory potential of the antigen-antibody reaction. Its use in the complex treatment of psoriasis is used by dermatologists with good effect. Aminasine in the form of 2.5% solution of 1 ml in 3 ml 0.5% solution of novocaine 1 - 2 times a day or orally 0.025 - 0.05 g 2 - 3 times a day after meals for 2 weeks is used. The use of aminazine is contraindicated in diseases of the liver, kidneys, expressed atherosclerosis, thromboembolic disease and the propensity for allergic diseases. Complications and side effects of the drug include dyspeptic disorders, reduced appetite, constipation, orthostatic colitis. With prolonged use may be leukopenia, agranulocytosis, hepatitis.
Sedatives and tranquilizers are widely used in psoriasis patients. However in practice it is impossible to be convinced of efficiency and effectiveness of these methods. In addition, having accurate data on the presence of deep, multifactorial metabolic defects in psoriasis patients due to the reduction of enzymatic and metabolic processes, overeating, hypodynamy and endocrine insufficiency, it is proposed to use sedative therapy or tranquilizers only temporarily and only in the presence of pronounced neurotic reactions and if novocaine, aminazine and antihistamines with sedative effect were not effective enough. In these cases, magnesium sulfate is used, which, in addition to sedative and hypotensive effect, has a laxative, choleretic and tonic effect. Especially shown magnesium sulfate psoriasis patients with obesity, impaired liver function, gallbladder, as well as patients with hypertension, intestinal atony, vascular spasmophilia of the skin. Magnesium sulfate is injected parenterally: intramuscularly or intravenously in the form of 25% solution in 3 - 5 - 7 - 10 ml per day - two taking into account the value of blood pressure for 20 - 30 days. In patients with obesity, insufficiency of thyroid function, it is most advisable to use magnesium sulfate inside 10 - 20% solution on a tablespoon 2 - 3 times a day for 2 - 3 weeks. As a sedative, normalizing and lengthening physiological sleep in patients with psoriasis is advisable to prescribe sibazone, seduxen, relaxium, phenazepam, nosepam, tazepam - 1 tablet at a dose of 0.005 g 1 - 2 times a day. Positive result in the treatment of progressive stage: psoriasis is noted when adding to the complex of anti-inflammatory lipotropic drugs in combination with beauty alkaloids and phenobarbital.
These include bellatamine, bellaspond, bellloid. To non-specific antipsoriatic drugs with a broad pharmacotherapeutic effect include vitamins that actively affect metabolic functions. It is known that the vital need for vitamins is due to their participation in the construction of many enzymes, which provides the regulation of metabolism, adaptive and trophic mechanisms, immunocorrective action. To treat psoriasis widely used vitamins complex B, especially B1, B2, B6, B12, B13, B15, vitamins A, E, C, P in combination with other therapeutic agents. Inclusion of vitamin B1, and even better than its coenzyme - cocarboxylase, in the complex therapy of psoriasis contributes to the regression of dry elements. Cocarboxylase is especially important for the regulation of carbohydrate metabolism, functional activity of the nervous system, endocrine glands and cardiac activity. Cocarboxylase is a ready form of coenzyme formed in the body from thiamine (vitamin B1). It is injected subcutaneously, intramuscularly or intravenously by 0.05 - 1 g once a day, every day, on a course of 10 - 15 injections. Contraindications - Hypersensitivity, allergic diseases, hypertension.
Vitamin B2 - riboflavin is part of the enzymes that regulate redox processes, is involved in carbohydrate, protein and fat metabolism, is necessary to maintain normal visual analyzer function. To treat psoriasis used 1% solution of riboflavin mononucleotide, administered intramuscularly to 2 ml a day, a course of 10 - 15 injections. Contraindications are idiosyncrasy and perforation. No complications in the use of riboflavin is observed. It is very advisable to prescribe vitamin B5 - calcium pantotenate, which is part of coenzyme A, which participates in the processes of acetylation and is one of the most important coenzymes of complex enzymatic systems of oxidative decarboxylation of pyruvic and a-ketoglutaric acids. In the process of acetylation during oxidative decomposition of carbohydrates, fats and proteins under the influence of vitamin B5 the metabolism of tricarboxylic acids is normalized - the central metabolic process of the cellular level.
Calcium pantothenate is used orally 0.1 - 0.2 g 3 - 4 times a day, as well as intramuscularly as 20% solution of 1 - 2 ml 1 - 2 times a day for 2 - 3 months. Contraindications - individual intolerance. Complications in the form of allergic reactions, dyspeptic events are extremely rare.
The positive effect in psoriasis has vitamin B6 - pyridoxine. Its coenzyme (phosphorylated) pyridoxalphosphate is necessary for decarboxylation and reamination of amino acids (tryptophan, methionine, cysteine, glutamine and other amino acids). By participating in the metabolism of fats and lipoproteins, it increases the excretion of cholesterol and triglycerides.
Pyridoxalphosphate is injected intramuscularly at 10 µg daily or 1 month later. Pyridoxine is used orally in powders or tablets of 0.025 g 3 - 4 times a day or as a 5% solution of 1 - 2 ml intramuscularly every day. The course of treatment lasts 3 - 4 weeks. Complications - allergic manifestations in the form of dermatitis or hives are rare. Contraindications - idiosyncrasy. Vitamin B12 (cyanco-balamin) is widely used in the treatment of psoriasis, as it participates in the synthesis of labile methyl groups, choline, methionine, nucleic acids, has a beneficial effect on the functional status of the liver and nervous system. It has a pronounced antianemic effect, normalizes the metabolism of carbohydrates and fats. The drug is administered intramuscularly from 50 to 400 mkg once a day. The duration of treatment is 1 month. Contraindications are thrombophlebitis, angina, erythrocytosis, violation of the rheological properties of blood. Complications of vitamin B12 use include allergic dermatitis, urticaria, swelling of Quincke, palpitations, erythroleukocytosis, nervous agitation.
Vitamin B13 - orotic acid is one of the precursors of pyrimidine nucleotides, which are part of nucleic acids that are involved in the synthesis of protein molecules. Orotic acid and its salts are considered as substances of anabolic action and are used in violation of protein metabolism and as common stimulators of metabolic processes. In dermatology, potassium salt of orotic acid (potassium orotate) is used. Take potassium orotate inside for 1 h before meals of 0.25 - 0.5 g 3 times a day. The course of treatment 20 - 40 days. Repeated courses are appointed after a monthly break.
Vitamin B15 (pangamatic acid and its derivative - calcium pangamate) is used to treat psoriasis, especially in erythrodermy or psoriatic arthropathy, in order to normalize lipid metabolism, rational absorption of acid-like tissues, increase energy resources of muscles and liver (creatine phosphate and glycogen), as well as to partially block pathological nerve impulses from the skin to the CNS. Due to the presence of calcium molecule, vitamin B15 has a significant anti-inflammatory and hyposensitizing effect. Calcium pangamate is administered orally to 0.05 - 0.1 g in the form of powders or tablets 3 - 4 times a day for 20 - 40 days, followed by a break of 2 - 3 months. It is contraindicated for glaucoma, hypertension. Side effects are rare, mainly in elderly people in the form of insomnia, headaches, irritability, tachycardia, extrasystole. Good therapeutic effect is noted in the treatment of psoriasis with folic acid, especially in patients with long duration of the disease in hospital, while in the period of exacerbation of therapeutic effect is little pronounced. Folic acid together with vitamin B12 stimulates the process of erythropoiesis, is an integral part of coenzymes, which carry out the synthesis of methionine, serine, choline, uracil, thymine, purine and nucleic acids. To treat psoriasis is prescribed orally 0.01 - 0.03 g 3 times a day 20 - 30 days in combination with vitamin B12.
In the treatment of various forms of psoriasis is widely used ascorbic acid (vitamin C), which is involved in the regulation of redox processes, promoting the synthesis of steroid hormones, collagen formation, cell membrane thickening capillaries. Psoriasis patients are prescribed ascorbic acid in 5% solution in 2 - 3 - 5 ml 1 time a day for 1 month in tablets or powders of 0.05 - 0.25 g 3 - 4 - 5 times a day after meals for 30 - 40 days. Ascorbic acid has a hyposensitizing effect, especially with intramuscular administration.
In the summer form of psoriasis and patients with severe fat metabolism disorder, it is advisable to prescribe nicotinic acid, which takes part in redox processes, reduces the content of cholesterol, triglycerides in the blood, has a positive effect on lipid metabolism and has a vasodilating effect. For the treatment of psoriasis nicotinic acid is used in a dose of 0.05 - 0.12 mg 2 - 3 times a day inside or as 1% solution of 1 - 2 ml subcutaneously or intramuscularly for 15 - 20 days. The contraindication may be individual intolerance. Prescription of nicotinic acid in severe forms of atherosclerosis, hypertension is sharply limited. Side reactions are manifested in redness of the face, upper torso, dizziness, a sense of the tide, paresthesia.
Vitamin D2 is used, which regulates the exchange of phosphorus and calcium, promotes the consolidation of cell membranes, has a positive effect on regenerative processes in the epidermis, contributing to the deposition of dehydrocholesterol in the skin. Apply vitamin D2 at the rate of 2000 IE per 1 kg of body weight, which averages 80000 - 160000 IE per day for 20 days. If tolerated well after 7 - 10 days of reception repeated and continue for 2 - 3 months. until the disappearance of clinical manifestations of psoriasis. Then taking vitamin D2 continues for a year with a monthly break after each month of treatment. Vitamin D2 is contraindicated for active forms of lung tuberculosis, gastric ulcer, duodenal ulcer, liver and kidney diseases, and organic heart and vascular diseases. Common side effects are dyspeptic symptoms, polyuria, hyperthermia, diarrhoea, internal calcinosis.
Violation of keratinization in psoriasis was the basis for the use of vitamin A or retinol. This vitamin promotes growth and development, provides keratogenesis processes in the epidermis. It has the property of maintaining the function of keratinocytes of the epidermis due to the normalization of plastic metabolic processes in the skin and mucous membranes. Retinol increases the absorption of proteins, fats and carbohydrates by intensifying redox processes and the synthesis of cholesterol, which is necessary for the construction of steroid hormones, enhances phagocytosis and the synthesis of protective antibodies. With vitamin A deficiency keratinization of the epidermis occurs, manifested by dry skin, flaking and cornification of the follicular apparatus. Xerophthalmia or keratomalacia may develop, so vitamin A (retinol) is called antioxerophthalmic, anti-infection. Appoint it inwardly to 10000 - 30000 IU per day 10 - 15 minutes after meals. Intramuscular administration of vitamin is rarely due to local soreness and possible formation of infiltrates. When taking large doses of vitamin A may be exacerbation of hepatocholecystitis and chronic pancreatitis, as well as irritability, drowsiness and hyperkeratosis of the hair follicles.
Treatment of common pustular, arthropathic psoriasis and psoriatic erythrodermia with tigasone is very successful. Tigazone is administered orally at the rate of initially 1 mg per 1 kg of body weight per day, and then after 2 - 4 weeks. dose is reduced to 0.75 - 0.5 mg/kg. The duration of treatment varies from 1 to 6 months. According to most authors, clinical recovery is observed in 70-80% of cases. The maintenance dose was 0.25 - 0.3 mg/kg per day.
Of the side symptoms are more often found dry mucous membranes, heilitis, focal, and sometimes total hair loss, paronias, petechiae, vomiting, hepatitis. All these complications are reversible and quickly disappear after the drug withdrawal. In order to reduce the single and total doses of retinoids, they are prescribed in low doses - 0.3 - 0.5 mg/kg per day in combination with PUVA-therapy, UVO and external application of corticosteroid ointments. This combination provides as good a therapeutic effect as high doses of retinoids. At the same time, the probability of various side effects and complications is significantly reduced.
Vitamin E (tocopherol acetate) stimulates cell metabolism by participating in the biosynthesis of DNA, RNA and tissue respiration. Vitamin E is a natural antioxidant and protects the metabolic processes of fats, proteins and steroid hormones from pathological oxidation reactions that are not associated with energy conversion and storage. Vitamin E is prescribed inside and intramuscular. For oral administration 5, 10, 30% oil solution of tocopherol acetate. In 1 ml contains 50, 100 and 300 mg of synthetic a-tocopherol acetate, respectively. Psoriasis patients are prescribed vitamin E from 15 to 100 mg per day for 20 - 40 days. Intramuscular injections due to painfulness and the possibility of infiltration is rarely prescribed. For injections, the drug is available in 1 ml ampoules containing 5, 10 or 30% solutions. For the treatment of psoriasis is prescribed a drug containing in 1 ml 5% or 10% solution, ie, 50 - 100 mg a day or 2 - 3 times a week, a course of 10 - 12 injections. Since vitamin E is a synergistic of vitamin A and potentiates its action, a complex preparation aevit, containing in 1 ml of acetate (vitamin A) acerophthol 35 mg - 10000 ME and a-tocopherol acetate (vitamin E) - 100 mg is used. Apply aevite orally in capsules of 1 ml 1 - 2 times a day with meals 20 - 40 days or intramuscular (slightly heated) 1 ml 1 time a day after a day, for a course of 15 - 20 injections.
Vitamin F is conditionally referred to vitamins. It consists of a complex of unsaturated essential fatty acids - liyolenic, linoleic and arachidonic. Unsaturated fatty acids have a significant impact on the functional activity of hepatocytes of the liver, taking part in the exchange of lipids, carbohydrates, mineral salts.
Unsaturated fatty acids are contained in linetool, a preparation derived from linseed oil. It has been established that in patients with psoriasis with hypercholesterolemia the content of cholesterol in blood serum decreases, the cholesterol/phospholipids ratio decreases, the content of b-lipo-proteins of low and very low density decreases. Lynetol is administered orally 1 tablespoon in the morning immediately before meals or during meals once a day for 1 - 1.5 months with breaks of 2 - 4 weeks. The linetol is transferred without side effects or complications. Contraindications are colitis, enterocolitis and hepatocholecystitis.
In recent years, more vitamin preparations with coenzymatic properties are used. These include phosphadenes and dipromonium. Phosphaden is one of the active adenyl nucleotides. As part of the coenzyme (flavine-deniny nicotinamiddinucleotide), phosphaden has hepatotropic effect, activates the processes of microcirculation, regulates the content of common lipids, free fatty acids and blood b-lipoproteins, and also takes part in the biosynthesis of protein and restores the synthesis of ATP. Dipromonium is a synthetic analog of vitamin B15. Metabolic effect of dipromonium is caused by improvement of liver functional state, lipid metabolism, increase of endothermic reactions activity with normalization of redox processes and microcirculation in peripheral ischemia syndrome.
Significant increase in the number of vitamin resistant forms of psoriasis, high incidence of severe forms of disease in the form of erythrodermic, arthropathic and other clinical variants of dermatosis required the introduction of highly effective methods. Corticosteroid preparations (hydrocortisone, prednisolone, triamcinolone, kenakort, etc.) are widely used. Different corticosteroids have a common therapeutic effect. The most pronounced are their anti-inflammatory and immunosuppressive effects, anti-neoplastic and hyposensitizing effects. With the introduction of fluorine-containing corticosteroid drugs it became possible to more reliably and quickly suppress the inflammatory reaction and achieve regression of psoriatic rash. Triamtsinolone and polkortolone proved to be especially good due to their epidermotropic action. These drugs were more effective in patients with generalized, disseminated psoriasis in the progressive stage. In the long term, in the presence of elderly foci or in patients with erythrodermia or arthropathy, the effect is slower, and in order to obtain clinical recovery requires increasing doses. When doses are reduced or when drugs are cancelled, the disease is almost continuously and rapidly exacerbated or relapsed (withdrawal syndrome). Clinical remission in this case requires already higher doses, causing complications and side effects. In addition, patients who have received hormones are resistant to other drugs. As a result, the use of corticosteroid hormones is increasingly restricted. They are used in complex therapy, mainly for severe forms of dermatosis such as psoriatic erythrodermy and arthropathic psoriasis. Of the currently available arsenal of hormonal drugs most often used prednisolone and its derivatives - urbanization, methipred, as well as triamtsinolone, dexamethasone, polkortolone, kenalog as the most effective and proven positive.
Prednisolone and its analogues - urbanization, methiipred prescribed internally, intramuscular and intravenously. When administered orally, the drug is used carefully, starting from 16 mg per day. The duration of treatment depends on the nature of the disease, the patient's condition and therapeutic effectiveness of the drug. Treatment is discontinued gradually, reducing the dose under control of its effectiveness. In acute cases, treatment is carried out intensively, using intramuscular and intravenous (jet or drip) injection methods. Prednisolone in 1 - 2 ml (30 - 60 mg), urban - 20 - 40 mg, methylred is administered intramuscularly (prolonged preparation) in 1 - 3 ml (0.04 - 0.13 g) once in 1 - 4 weeks.
Polkrtolone and kenalog are effective in psoriasis patients due to epidermotrope action. Polkrtolon is administered orally 4 - 8 - 16 mg in 2 - 4 doses, after the therapeutic effect is reduced by 1/3 - 1/2 tablets until a minimum maintenance dose - 0.001 g per day. Kenalog is produced in tablets of 0.004 g and in ampoules containing 1 ml 40 mg of tramcinolone acetonide. When taken orally, prescribe initially 4 - 6 tablets a day. With a positive therapeutic result, the dose is gradually reduced to a maintenance dose, after which it is possible to switch to a maintenance equivalent dose of kenalog-40, which has the deposit ability with gradual absorption. Intramuscular injections of kenalog-40 are made once in 2 - 3 weeks. In patients with severe forms of psoriasis it is necessary to use kenalog-40 intramuscular at once without taking tablets and to increase the dosage up to 80 mg per week for vital indications.
Dexamethasone, or dexazone, is fluorinated methylprelnisolone, which has a more active anti-inflammatory and anti-allergic effect. In terms of efficiency, 0.5 mg of dexamethasone corresponds to approximately 3.5 mg of prednisolone, i.e. it is 7 times more active than prednisolone. Inside dexamethasone is prescribed in 2 - 3 doses of 2 - 3 mg per day during or after meals. Parenterally (intravenously or intramuscularly) is prescribed in severe cases 1 - 2 ml (0.004 - 0.008 medication once a day).
In the process of glucocorticoid treatment side effects and complications are possible, especially often occurring with prolonged prescription. Along with anti-inflammatory and anti-allergic they have immunodepressant, cytostatic action. At the same time they manifest themselves as a catabolic mechanism of metabolic reactions with the release of potassium and calcium and sodium retention in the tissues, which leads to muscle weakness, activation of infection, swelling, obesity of the type of Itsenko - Cushing syndrome with the presence of hypertension. Glucocorticoids stimulate the increased formation of glucose and contribute to the formation of true diabetes, lead to the development of gastric or intestinal ulcer, osteoporosis (more often in the spine), increased CNS excitability, resulting in insomnia, increased irritability, euphoria. Corticosteroid hormones are contraindicated for patients with diabetes, infectious diseases, hypertension, epilepsy. To prevent catabolic complications, corticosteroids are administered in combination with anabolic drugs such as nerobol (methandrostenolone, methylandrostendyol) - 0.005 g 2 times under the tongue for 20 - 25 days. Prolonged medications (phenobolin, retabolil) are injected intramuscularly 1 time in 7 - 10 - 15 days for 50 mg. In order to normalize mineral metabolism inside prescribe potassium (panangin, potassium orotate), calcium (calcium chloride, gluconate, glycerophosphate), sodium chloride (table salt) is limited. At the same time limit fats and carbohydrates, and in the food added protein and vitamins (calcium pantothenate, aevitis).
Along with hormones, cytostatic preparations (methotrexate) are also used. However, the proximity of its therapeutic and toxic doses contributes to numerous complications. Often observed hepatitis, dyspeptic phenomena, erosive foci on the mucous membrane of the mouth, oppression of hemopoiesis, hemorrhagic syndrome. However, side effects quickly disappear after the drug withdrawal.
Better tolerability of methotrexate promotes the additional use of small doses of corticosteroids, vitamins, immunostimulants The combination of fractional methods of methotrexate with immunomorrectors such as sodium nucleotide, decaris allows you to sharply reduce hepatotoxicity, improve the effectiveness of treatment of scaly deprivation until a clinical cure. In addition to methotrexate, in the treatment of psoriasis, other cytostatic agents are used to inhibit the growth factor of keratinocytes proliferation and inhibit enhanced protein synthesis and metabolism of nucleic acids.
Antimetabolic drug - hydroxyurea (hydroxyurea, biosupressin) - is also used in the treatment of psoriasis and quite widely. The reason for this is its sufficiently high efficacy and lower side effects compared to methotrexate and other cytostatics. However, the revealed changes in sexual chromatin indicate the need for careful use of this drug in the treatment of young people.
In the treatment of psoriatic arthritis for many years used non-hormonal anti-inflammatory drugs - brufen, indomethacin, butadione, Voltaren, methindol, samecylates. Their distinct therapeutic effect and good tolerability have been established. These anti-inflammatory drugs stabilize the membranes of lysis, depress the intensity of proliferative inflammatory reactions, increase energy supply of metabolic and immune processes.
It hasn't lost its significance in the treatment of psoriasis pyrotherapy. The increase in body temperature is a powerful factor mobilizing the phagocytic activity of leukocytes, the synthesis of interferon, protective reactions of the reticuloendothelial system and the function of the pituitary adrenal adrenal system. Hyperthermia may be caused by pyrogenic injections. Pyrogenal is used for pyrotherapy, which is recognized for its lack of sensitizing properties. Pyrogenal is a bacterial pyrogen obtained as a complex protein-free lipopolysaccharide complex from the culture of synergistic and abdominal mycobacteria. The pyrogenal is injected intramuscularly at 25 - 60 minimum pyrogenic doses in gradually increasing quantity to 100 - 150 minimum pyrogenic doses per injection in a day or 2 times a week. The course of treatment is 10 - 12 injections.
Adaptogens are successfully used in the treatment of psoriasis: aloe liquid extract, lemongrass tincture, lure tincture, levza liquid extract and eleutherococcus liquid extract. Despite the numerous possibilities of psoriasis therapy, the process usually remains long, often relapsing. In order to influence the various pathologically altered mechanisms of metabolism, hemodez, a hemostatic substitute with a pronounced detoxifying effect, is used. The preparation in the amount of 300 - 400 ml is injected intravenously at a rate of 80 - 100 drops per minute at intervals of 3 - 4 days, for a course of 5 - 8 injections.
It is worth noting the use of heparin, especially in the treatment of severe forms of psoriasis. Studies on the use of heparin stated immunodepressant, cytostatic, anti-inflammatory effect of heparin. Heparin is injected subcutaneously into the abdominal area, starting from 5000 units 4 times a day for 7 - 10 days, then 2 times a day also 7 - 10 days, and then as a maintenance dose once a day in the amount of 10 - 15 injections.
Phosphodiesterase inhibitors are widely used in medical practice. These include methylxanthin group drugs - theophylline, euphylline, caffeine, trental, papaverine, ATP and some antihistamines (tavegil, fenkarol, diprazine).
In the dynamics of the course of psoriatic disease every year there are changes in the direction of prolongation and burdening of the process, so there is a further search for new, more effective methods.
Means of external therapy. In the treatment of patients with psoriasis has long been widely used ointments, taking into account the stages of the process, as the local therapy improves the effectiveness of drug treatment. In the progressive stage is often used 2% salicylic ointment, boron-salidol ointment (Rybakov ointment), lanoline-water cream Unna. With a pronounced inflammatory process with exudative component prescribed ointments and creams with corticosteroid hormones. Good anti-inflammatory, anti-allergic and resorptive effect of ointments such as flucinar, deperzolone, oxycourt, Lorinden C, Lorinden A, and others. To accelerate the healing effect in patients with psoriasis psoriasis corticosteroid ointments are applied after removal of scales and crust 2% salicylic or sulfur salicylic ointments. In areas of severe infiltration, in the area of large plaques ointments are applied under the bandage. A complete cure of psoriasis is not achieved. However, ointments or creams with corticosteroids are shown in all stages of psoriasis and especially in the period of progressive flow. In the stationary and regressive stages, tar and sulfur-degty ointments, 5 - 10 and 20% ichthyol, 5 - 10% ichthyol-naphthalanes are recommended. Efflorescence regression is especially accelerated when tar, ichthyol or naphthalene ointments with corticosteroid ointments are combined. It is advisable to change ointments, as often there is a "getting used" of the skin to the same ointment. Especially necessary change of means of external therapy in a regression stage, when it is necessary to intensify resorption of infiltration of plaques. In the absence of fresh eruptions can gradually increase the concentration of active components of ointments and creams. The prescribed ointments are 2 - 5 % white mercury ointment, 0 - 15 % sulfur-degree ointment, 20 - 33 % sulfuric ointment, Wilkinson ointment, 0,5 - 10 % chrysorosebin ointment, 0,5 - 1 % cignoline (dioxyanthranol), Anthramium or Psoriasin and Antipsoriatic ointments, which have not only exfoliating and anti-inflammatory, but also reducing and plastic action.
Local treatment of patients with psoriasis with sulfuric, tar, salicylic ointments, especially in common processes, requires constant monitoring of kidney function. In addition to the toxic effects, tar ointments cause folliculitis in some patients, which is an indication for their elimination. Significant therapeutic effect is also observed in the use of ointments with methylxantine compounds: 5 - 10% theophylline, 2 - 5% euphylline and 2 - 5% papaverine ointments and creams.
Attempts have also been made to treat psoriasis with ointments containing antiviral agents. Tebrofenovaya, oxolinovaya, bonaftonovaya (1-2-3%), as well as 1-3% interferonovaya and 2-5% alpizarinovaya ointments are prescribed. These ointments help to resolve rashes, especially in small papule efflorescences, and they are well tolerated by patients and do not cause side effects. In order to accelerate the resolution of psoritic elements, the use of tar, ichthyol ointments is combined with UVO. In this case, UVB rays not only accelerate the resolution of inflammatory foci, but also prevent the development of dermatitis from these ointments in cases where they are prescribed in a significant concentration (5 - 10 - 15%).
Due to the presence of metabolic disorders in psoriasis patients, manifested by both quantitative shifts in the content of cholesterol, carbohydrates, proteins, trace elements and vitamins, and significant enzymatic pathological conditions, it is considered advisable to regulate the diet, limiting the consumption of food containing animal fats and proteins, carbohydrates and spices. It is also important to harden the body, increase mobility and mobility in the form of therapeutic exercise or sports.
Promising methods of treatment. In recent years there have been significant improvements in psoriasis treatment methods. In addition to traditional schemes and methods, active efferent methods based on detoxifying and immunocorrective effects are being developed. In connection with in-depth virological studies are expanding indications for use of a complex of antibiotics with antiviral agents. Indications for use of cytostatins and immunosuppressive drugs have been narrowed. Corticosteroid hormones for general therapy are administered with care and restraint, and their local use is limited.
Already in the first years after the introduction of corticosteroids revealed their negative properties. With dose reduction and drug withdrawal almost always and very quickly there is a relapse. A significant increase in dose, accompanied by complications and side effects, is required to control exacerbation. It should be especially noted that patients who received corticosteroids, relapses more quickly, resistant to other therapies. With the use of corticosteroid hormones associated increased incidence of severe course pustular psoriasis.
Based on the data obtained from the study of the results of photochemotherapy, it became known that this method is one of the most effective for psoriasis. However, short terms of clinical remission in many cases as well as frequent side effects and complications testify to the necessity to shorten the terms of treatment and apply photochemotherapy as a component of combined scheme in combination with efferent methods or use selective phototherapy.
Wide introduction of efferent methods into the practice of dermatosis treatment is the result of many years of searching for effective methods of struggle with endogenous toxic factors changing the homeostasis system. A characteristic feature of efferent therapy is the elimination (removal) of xenobiotics from the body by various methods. For removal of autotoxic products of metabolism from the body such primitive methods as prescription of vomiting and laxatives, bloodletting, forced diuresis have long been used.
Currently, such advanced detoxification methods as hemodialysis, hemosorption, hemofiltration, ultrafiltration and plasmapheresis have been developed.
Psoriasis patients, especially those with severe chronic forms, are overloaded with pathological immune circulating complexes, blockage, depression of physiological systems of protection and regulation, functional disorders of gastrointestinal system. All this causes the development of endogenous intoxication syndrome, as a result of which the body accumulates an excessive amount of intermediate and final metabolites, which have a toxic effect on the functional state of the most important systems. Efferent methods have a detoxifying systemic effect, in which the removal of xenobiotics and various toxic factors leads to non-drug stimulation of natural immunity systems, physiological mechanisms of sanogenesis with normalization of life processes.