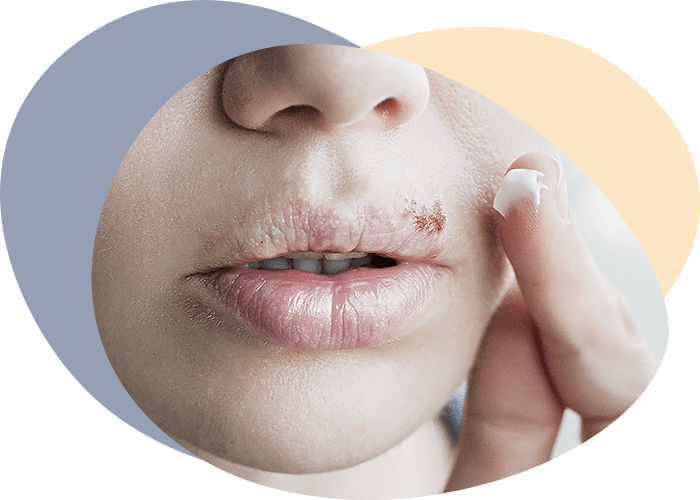
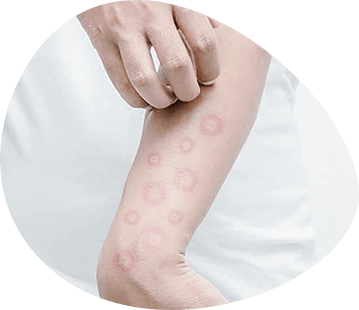
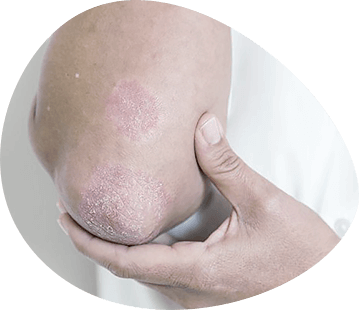
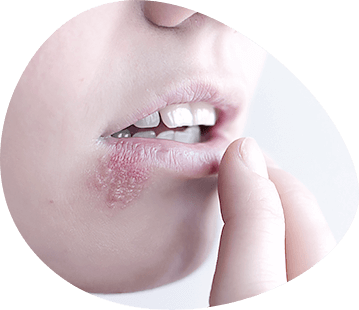
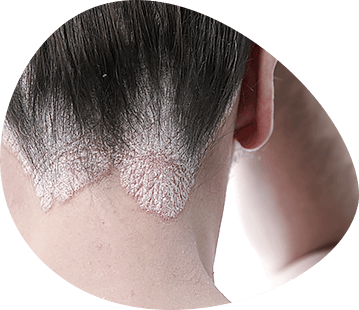
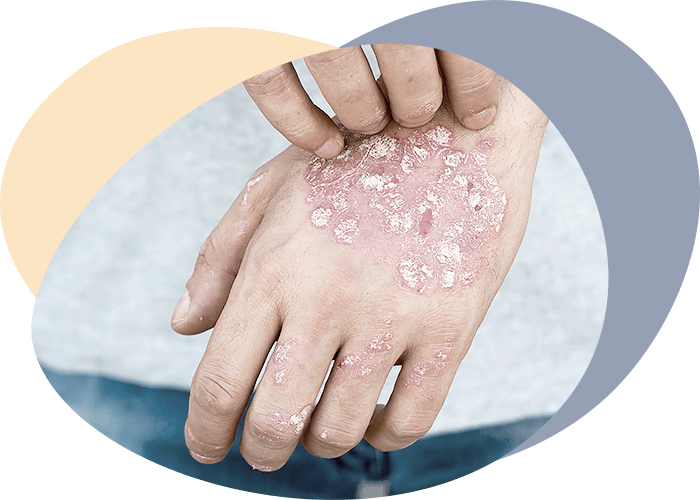
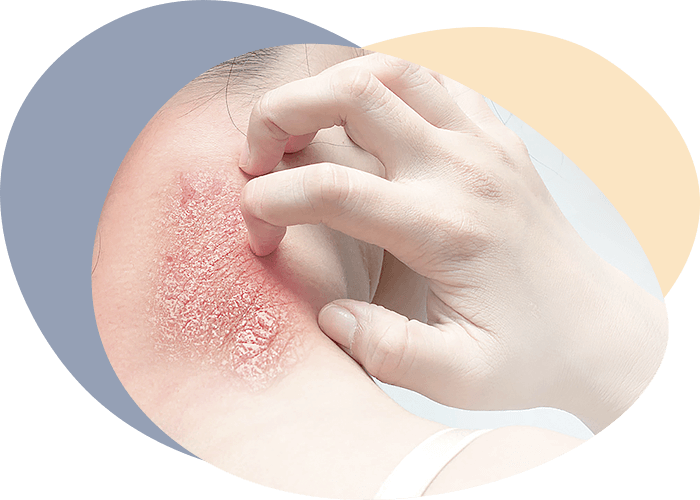
The mucous membrane of the mouth and the red edging of the lips are the site of a large group of dermatoses. The diagnosis and treatment of oral mucous membrane lesions in dermatosis should be done in conjunction with dermatologists and other specialists.
Red flattened lichen (RFL) is a chronic disease that affects the covering tissues; it is clinically manifested on the skin and mucous membranes. Oral mucous membrane lesions with red flattened lichen may be combined with skin lesions, but are often isolated. Among oral mucous membrane diseases, red flattened shingles are the most common (50-75%). Women aged 30 years and over are predominantly affected.
Etiology
The etiology of the disease is not definitively clear. Some authors attribute red flattened herpes to autoimmune diseases, in the initiation of which a significant role belongs to the cells of Langerhans, supplying T cells of autoantigenes and producing a number of anti-inflammatory cytokines.
To date, there are several theories of red flattened lichen:
- Inheritance theory There have been cases of family illness and manifestations of oral mucous membrane RFL in twins.
- Infection theory (confirmed by single cases during observations).
- Role of drugs, physical and chemical factors.
The arsenal of products that can cause RFL has expanded significantly: gold, arsenic, mercury, vitamins, antimalarial drugs, bromides, PASK, streptomycin, tetracycline, furosemide, sulfonamides, antiarrhythmic drugs and many others. Toxic-allergic defeat SOPR and skin of drug origin often occurs with a lichenoid reaction - the so-called medication RFL.
The condition of the oral cavity (injuries, poor quality prostheses, prostheses made of dissimilar metals, dysbacteriosis) is of certain importance.
- Neurogenic theory.
In 65% of patients there is a clear connection with emotional stress, nervous and psychological shocks, negative emotions, diencephalic crises, sleep disturbance, neuroendocrine regulation (early onset of menopause, hypoestrogenemia, hypertension). There is a certain connection between RFL and diabetes mellitus, in pathogenesis of which there is a disorder of the sympathetic-adrenal system.
- Endocrine and metabolic disorders.
The high frequency of combination of RFL with diabetes mellitus, especially in case of SOPR and atypical forms of RFL, indicate the commonality of their pathogenetic mechanisms and the role of endocrine exchange disorders, which gives grounds to highlight carbohydrate dysmetabolism in the characteristic feature of RFL.
- Immunological mechanisms of RFL development cause lesions of epithelium (epidermis) tissues and own plate by the type of late immunological reaction with cytotoxic effect.
Red flattened lichen occurs against the background of long-term diseases of the gastrointestinal tract, liver, pancreas. Especially severe course of the disease is observed in patients with calculous cholecystitis, cirrhosis of the liver, decompensated diabetes mellitus.
The clinic of red flat stripping in persons suffering from diabetes mellitus in combination with hypertension is called Greenspan syndrome. Thus, today RFL is seen as a multifactorial process in which the leading links of pathogenesis are neuroendocrine, metabolic and immune mechanisms.
Classification
In modern systematics 6 forms of red flat stripping on the mucous membrane of the mouth cavity and red edging of lips (according to Pashkov B.M. classification) are distinguished:
- typical,
- Hyperkeratotic,
- exudative-hyperemic,
- a erosive ulcer,
- bullous,
- Atypical.
However, in the practical work of a dentist most often there are 3 forms of the disease: typical, exudative-hyperemic and erosive- ulcer. The transition of one form to another is possible.
General clinical manifestations
The main pathomorphological element in all forms of red flat lichen is papula, but in the exudative-hyperemic form is also observed erythema stagnation, in the erosive ulcer form - erythema, erosion or ulcer, in the bullous form - blister, erosion, erythema, in hyperkeratotic - papula merge into plaques.
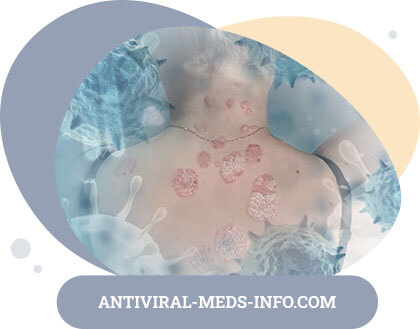
On the skin, the disease is manifested by rashes of polygonal papules in the forearms, shins, abdomen, chest and back. The papules are blue-red with a waxy shine. Their surface is smooth at first, then covered with grayish-white scales. The elements are often grouped, sometimes merged, but can be placed in isolation. The papules on the mucous membrane of the mouth cavity differ from those on the skin with smaller sizes, white colour, characteristic pattern of grouped elements, expressed exudative background, formation of erosions, ulcers, sometimes bubbles. Quite often rashes are poured out in isolation on the mucous membrane of the mouth and the red edging of the lips, and the skin and other mucous membranes are affected later when the pathological process becomes heavier and more progressive.
Two localizations are predominantly characteristic of the RFL of the oral mucous membrane:
- The most typical is the distal region of the cheek or retromolar region, where polygonal papules, merging with each other, form a pattern in the form of fern leaves or mesh, are clearly delimited and can be propelled;
- a tongue (dorsal and lateral surface) in which the signs of the disease are very diverse: polygonal nodules forming an area or cover with scarlike stripes, grids, atrophic areas of the mucous membrane, or hypertrophic papules.
A distinctive clinical picture has a RFL on the red edging of the lips. In most patients, rashes are represented by individual papules of small size, polygonal shape. Individual papules are grouped, connected to each other by keratinized bridges and slightly rise above the surrounding red border. The cornification of the papule tip gives them a whitish or whitish-gray colour.
In other areas of the oral mucous membrane, RFL is much rarer. When localized on the gums, the formation resembles a grid, wood, irregularly convex stripes, on the lips - starry stripes or spots; on the tonsils - small, dazzling white "cauliflowers".
Peculiarities of the disease flow
Red flattened herpes, being a chronic disease, may have different current activity, including on the oral mucosa, so distinguish between acute and chronic stages of the disease.
In the acute stage, in the typical form new papules appear, in the exudative-hyperemic form hyperaemia and exudation increase, in the erosive- ulcer form new erosions appear or increase in size. Any mucous membrane injury may provoke new eruptions or aggravate existing symptoms (a positive Kebner symptom is the appearance of new papules at the site of the injury).
In chronic steel, the Kebner symptom is negative, the process is not progressing, rashes may disappear periodically, but then appear again.
Pathogistological picture of red flat stripper is characterized by hyperkeratosis, paraceratosis, granullosis, acanthosis. Vacuum dystrophy of cells of the basal layer of the epithelium is sometimes observed. Under the epithelium there is a diffuse inflammatory infiltration, mainly of lymphocytes and plasma cells. Transformation of red flat lichen into cancer is accompanied by immersion of epithelial outgrowth into the subject connective tissue, disappearance of basal membrane, disassembly of basal and spiky cells, infiltrating growth with formation of keratinization zones of the epithelium. At the beginning of the transformation, one of its early signs is an increase in the number and size of nuclei.
Parkeratosis - incomplete cornification of surface cells of the spiky layer with the preservation of flattened elongated nuclei in them. In this process the phase of keratogialin and eleidin formation falls out, so there are no grainy and shiny layers. Keratin disappears from the cells of the corneal layer, so there is a pronounced peeling of the epidermis.
Acanthosis is a thickening of the epithelial layer of the mucous membrane due to proliferation of basal and studded cells. As a result, a nodule (papula) is formed.
Vacuum dystrophy - intracellular edema of epithelial cells with the appearance of vacuum in the cytoplasm, destroying cells. Vacuum can take up almost the entire cell, pushing the nucleus to the periphery.
Clinical picture of different forms of red flat stripping
Typical shape
This form on the mucous membrane of the oral cavity is the most favorable.
Interviews. No complaint or complaint about the feeling of tightness of the mucous membrane of the mouth, discoloration of the mucous membrane, roughness, sensitivity disorder in the focus of the lesion...
Anecdotal evidence. Neuroses, gastritis, colitis, diseases of the liver, pancreas, cardiovascular system, endocrine system. Sensitization to medicinal and chemical substances. The above mentioned diseases predispose to the development of RFL, while reducing the resistance of both the entire body and oral mucosa to various stimuli.
Skin: not changed, or on the bending surface of the forearms, wrist joints, inner surface of the thighs, the extension surface of the tibia are papules with a diameter of 2-3 mm, polygonal shape, pinkish-violet with a shiny surface and west in the center. When the papules are grouped together, a complex pattern is formed that is not repeated in different patients, it is called the "Wickham grid".
Pathogenesis: thickening of all layers of the epidermis, acanthosis, moderate hyperkeratosis, parakeratosis, irregular thickening of the granular layer (hypergranullosis). At the top of the dermis papillomatosis, inflammatory infiltration, consisting mainly of lymphocytes. Sometimes between the epidermis and dermis infiltrate are slotted spaces with gray content due to uneven thickening of the grain layer of the epidermis.
On the red edging of the lips: there may be no change or single or merged papules. The lesion area is mainly linear in shape, with dry lips and slight peeling. The mandibular and chin lymph nodes have not been altered, as there is no antipene stimulation of lymphatic cells.
On the oral mucous membrane, grayish-white papules ranging in size from 0.2 to 2-3 mm merge into a bizarre pattern in the form of lace, mesh, fern leaves (Wickham's mesh) and are located on the pale pink (less often on the stagnantly hypermolarized) mucous membrane of the cheeks, lips, retromolar region, and on the lateral surfaces of the tongue. The surface of the papules slightly extends above the mucous membrane level. The colour of the papules is due to cornification of the epithelium. Palpation of the papules is painless. On the mucous membrane of the tongue plaques are formed, which have the form of white fields ranging in size from 0.5 to 2 cm and more. There are no tongue papillae in these areas or their height is significantly reduced. The location of the papules in the area of the gums may be parallel to their edge. In the oral cavity and on the red edging of the lesion lips are usually symmetrical.
Pathogenesis: in the epithelial layer of the phenomena of acanthosis, parkeratosis, hyperkeratosis. In the papillary layer, inflammatory diffuse infiltration, lymphocytes predominate.
Differential diagnostics of the typical form of red flat lichen is carried out with leukoplakia, Fordyce granules, secondary syphilis, pseudomembranous candidiasis, sometimes with Bowen's disease, with red lupus.
Fordyce granules are yellowish nodules, sometimes they are sprayed in considerable quantities in the thick of the mucous membrane, but do not change its relief. In contrast to red flat lichen, there is no hyperkeratosis, inflammation of mucous membrane, sebaceous glands are covered with epithelium. The papules in secondary syphilis differ from the papules in red flattened shingles with large size, correct rounded silt with oval outlines; the white color of their surface is determined not by hyperkeratosis but by plaque and partially by epithelium necrosis, which can be removed at scraping. There is a large number of pale treponemas, Wassermann's reaction and sedimentary reactions are positive.
Pseudomembranous candidiasis resembles red flattened lichen only externally, as tiny plaque has white colour but no hyperkeratosis. The plaque is partially scraped off with a trowel and a large number of yeastlike fungi are found in the scrape.
The manifestation of Bowen's disease in the mouth is limited, the element of lesion is a spot, while the elements of lesion with red flattened lichen - papules are found in various areas of the mucous membrane and often in typical symmetrical areas on the cheeks, tongue. In difficult diagnostic cases, consultation with an oncologist is shown.
At red lupus also there is hyperkeratosis in the form of points, stripes, arcs, elements of lesion are located on the hypermised mucous membrane, in the center of the focus is determined by atrophy.
Flat leukoplakia occurs as a typical form of red flat stripper without complaints. The mucous membrane of the mouth cavity is unchanged, with elements of cornification of grayish-white colour. The element of lesion is a hyperkeratonic spot, usually a single one. It is located according to the trauma (sharp edges of the prosthesis, crowns). The mucous membrane of the anterior cheek and mouth catch is affected more often. The skin is not affected.
In leukoplakia, there is no inflammatory background around the lesion area and the mucous membrane under the lesion area has been changed with red flattened lichen. Hyperkeratosis prevails histologically, there is no acanthosis.
Exudative-hyperemic form
Complaints: sadness, itching, burning of the mucous membrane of the mouth, pain under the influence of various irritants (acute, irritating food. taking medicines, prosthetics, etc.). Chronic disease reduces the protective properties of the organism and the resistance of the oral mucous membrane. Functionally defective oral mucous membrane adsorbs the antigen (chemical, medicinal, microbial) and sensitizes. Its resistance to injury is reduced.
Complaints may also be about the roughness of the mucous membrane - these are cornifying papules.
Anamnesis. There may be an exacerbation of some comorbidities that contribute to the transition from a typical form to an exudative-hyperemic one. Lack of typical form treatment. Duration of the disease from several weeks to several months (according to the patient's subjective feelings).
Examination. The red edging of the lips is affected more often than in the typical form. This form has a more pronounced inflammatory reaction of the mucous membrane.
On the hyperemic mucous membrane of the cheeks, lips, bottom of the mouth, side surfaces of the tongue there are multiple gray and white papules up to 2 mm in size. The papules may be single or merge into bizarre patterns, but on a hyperemic background the "Wickham grid" is poorly visible. It becomes clearly visible after being lubricated with mucous iodine solution (Schiller-Pisarev's sample). Epithelial integrity disorders are not detected.
Palpation of regional lymph nodes is painless.
Often the development of exudative-hyperemic form is due to the addition of fungal infection.
Pathogenesis. The connective tissue layer of the oral mucous membrane is swollen, inflammatory infiltration is more pronounced than in a typical form. Significant lengthening of interosseous epithelial processes.
Differential diagnostics is performed with red lupus, acute atrophic candidiasis, Bowen's disease.
In the typical form of lupus erythematosus there are no papulosic elements, but there are areas of hyperkeratosis in the form of stripes, dots, and on the red edging of the lips - in the form of hyperkeratotic scales, which are located on a hypermised background, in the center of the lesion area atrophy is observed.
Localization of pathological elements mainly on the face skin. Development stages are typical: erythema, hyperkeratosis, atrophy.
Acute atrophic candidiasis is characterized by bright hyperemic, dry, painful oral mucous membrane with possible tiny white patches. Whitish formations are colonies of yeast mycelium, which merge, impregnate with fibrin and form coarse whitish-gray films in the long term. When scraping, the plaque is removed, revealing a hypermised or erosive surface. There is no openwork pattern from the papules on the mucous membrane. In macroscopic examination, a scrape from the mucous membrane is detected in large quantities of spore-forming cells of Candida fungus and mycelium filaments. In the history of prolonged antibiotics, glucocorticosteroids, cytostatics. It also develops in pharmacists who have constant contact with antibiotics.
Differential diagnostics with exudative-hyperemic RFL form complicated by candidiasis may be difficult. Anamnesis and trial antifungal treatment make it possible to clarify the diagnosis. After antifungal therapy, this form of RFL becomes typical, and acute candidiasis is completely curable.
Bowen's disease can be masqueraded as RFL by the appearance of cornification sites, but with RFL you can always find individual papules, typical "Wickham's net" in typical oral mucous membrane sites.
Erosive ulcer form
Complaints: acute painful rashes on the mucous membrane of the mouth (erosion). Constant pain and burning of the mucous membrane of the mouth makes it difficult to speak and eat. Pathogenesis: the integrity of the epithelium is impaired. Inflammatory exudate in the mucous membrane itself, inflammatory mediators, toxins, chemical factors irritate the nerve endings of the oral mucous membrane.
Past medical history: the duration of the disease from a few days to several years after the onset of oral pain. It is long lasting, progressing as a complication of typical, exudative-hyperemic and other forms, sometimes malignant (1%).
Prevailing factors: stress situations, exacerbation of background diseases, medications, oral mucosa injuries, prosthetics. Weaken the body's protective properties, reduced resistance of the oral mucous membrane to trauma and its regenerative capacity.
The recurrence of erosions is uncertain, from several weeks to several years. It depends on the general condition of the body, the treatment of concomitant diseases, the impact of provoking factors.
Efficiency of treatment: difficult to treat. The effect is achieved gradually, after several weeks of complex treatment: hyperemia of the oral mucous membrane disappears, erosions are epithelized (transition to a typical form). Treatment is effective with the right choice of methods and means of pathogenetic therapy, treatment of related diseases.
External examination . The submandibular and chin lymph nodes are soft, mobile and can be slightly enlarged.
On the mucous membrane of the mouth on a hyperemic background of irregular shape sharply painful erosions of various sizes, from dotted to extensive, covered with dense fibrinous plaque, against the background of the characteristic papulegic pattern (lace, mesh and p.) flat stripper.
Pathogenesis: Fibrin, lymphocytes, plasmocytes predominate in inflammatory exudate. Vacuum dystrophy of basal soybean epithelium. In the epithelial layer of acantholysis, hyperkeratosis, granullosis. Violation of the integrity of the epithelial cover. The connective tissue layer of the mucous membrane is swollen, capillaries are dilated, inflammatory infiltration is sharply pronounced, interosseptic spurs of the epithelium are lengthened.
Differential diagnostics with multiform exudative erythema, red lupus, vesicle, allergic stomatitis.
Allergic stomatitis begins acutely. It is accompanied by an ailment, an increase in body temperature, which is associated with taking medication, hyperemia and swelling of the mucosa.
Mucous membrane swelling is pronounced. Erosion is quickly epithelized (4 - 10 days). No papules. Does not relapse if allergen contact is excluded. Positive skin samples with allergen and allergic tests. Histologically in the focus - lymphocytes, plasmocytes, eosinophils, neutrophils, fat cells.
The benign vesicle is more often localized on the alveolar gum and the transition fold. Friction of the mucous membrane causes the formation of hemorrhagic or serous bladder in the corresponding area. No papulegic elements Common signs are: complaints of mucous membrane soreness, making it difficult to eat. On hyperemic mucous membrane erosions of irregular shape, covered with plaque, painful, easy to bleed when scraping.
Red lupus. As with flattened shingles, patients may complain of persistent pain in the mouth, intensified by irritants. On the hyperemic mucous membrane areas of corneal epithelium, erosion, ulcers of various sizes and shapes, covered with fibrinous plaque. When plaque is removed, bleeding appears. Erosions or ulcers persist for a long time. Skin lesions may occur.
Affection of the mucous membrane of the mouth is usually preceded by characteristic erythema spots on the skin (more often the face, red edging of the lips). Sunlight serves as a provoking factor, as patients have a sharply increased sensitivity of the skin to sunlight. Around the erythema erosion, there is a white striped, thin, radially diverging from the centre of the focus (peculiarities of cornification). At the periphery, the cornification phenomenon intensifies, forming a slightly elevated edge. After healing of erosions, atrophic scars remain.
Hotspots of cornification with red lupus on the mucous membrane of the mouth in the rays of voodoo glow snowy-blue or snow-white. DNA deposits in the basal membrane are detected by the RIF method. Parkeratosis, hyperkeratosis, vacuum degeneration of cells of the basal layer, degeneration of collagen fibers, periovascular infiltration from lymphocytes, proliferation of blood vessels are detected in histological examination.
Multiform exudative erythema is accompanied by significant hyperemia and edema of the oral mucous membrane, on the background of which there are irregularly shaped bubbles and erosions, covered with fibrinous plaque, sharply painful.
There are no papule rashes around erosions in multiform exudative erythema. Full resolution of the process on the oral mucosa takes 4-6 weeks.
Bullseye shape
Complaints: the formation of bubbles, mucous membrane pain, increasing with meals. Violation of the integrity of the epithelium due to rupture of the bladder tire. Inflammatory exudate, mechanical and chemical factors irritate the nerve endings of the mucous membrane of the mouth.
Examination: When examining the oral mucous membrane, the color of the oral cavity has not changed or the mucous membrane is slightly hyperemic. Bubbles 5 to 20 mm in diameter with turbid or hemorrhagic contents.
Multiple papules form a characteristic pattern (lace, fern leaves, etc.).
The exudate (bubble content) is located subepithelially. The round-cell infiltration is expressed in the mucous membrane itself. The capillaries are dilated. Diapaedesis of erythrocytes makes the content of the bladder bloody. In epithelium, irregular acanthosis, parkeratosis, vacuum dystrophy of the basal layer of the epithelium. The basal membrane can be destroyed by infiltration.
Differential diagnostics with vulgar vesicle, bullous pemphigoid, vascular-bubble syndrome.
In vascular-bubble syndrome, bubbles are formed as a result of trauma (friction) of the mucous membrane by prosthesis, food lumps, etc.. The content of bubbles is hemorrhagic. Anamnesis of cardiovascular disease, hypertension. It occurs, as a rule, in people over 40 years. Cytologically determined the accumulation of normal cells of different layers of the epithelium and neutrophils. Histologically - increased permeability (fragility) of the walls of small vessels, destruction of the basal membrane, which weakens the connection between epithelium and connective tissue layer of the oral mucous membrane.
Patients complain of mild pain in the oral mucous membrane. Subepithelial bladders occur on the unchanged oral mucous membrane and last from hours to days.
Direct and indirect RIFs are of great diagnostic value, which allows a clear differentiation of the vesicle and the bullous pemphigoid from the bullous form of flattened herpes. In addition, in vulgar vesicle smears taken from erosions, acantholytic cells are detected. In nonacantolytic vesicles, just like in the bullous form of flattening lichen, bubbles are formed under the epithelium, but around them there are never papule rashes.
Hyperkeratotic form
Complaints: on the roughness, an unusual type of mucous membrane of the oral cavity.
Elements of defeat - plaques, rise above the level of the mucous membrane. Hyperkeratosis is pronounced. In stroma is defined diffuse chronic inflammation with infiltration of lymphocytes and histiocytes, in the granular layer occurs acanthosis.
Past medical history: Bad habits and chronic trauma of the oral mucous membrane are detected. Duration of the disease - several months, years. Hyperkeratotic form develops as a complication of typical and exudative-hyperemic.
Prevailing factors: chronic mechanical trauma, prosthetics, bad habits, smoking, alcohol.
External examination. There may be typical skin manifestations. On the mucous membrane of the mouth cavity single areas of hyperkeratosis of various shapes and contours and clear boundaries on the background of typical papuletic elements.
Pathogenesis: inflammatory infiltration in own mucous layer, interepithelial papillae are elongated. In the epithelial layer of acanthosis, parkeratosis, marked hyperkeratosis, granullosis.
Differential diagnostics with verrucose form of leukoplakia, pseudoembranous form of candidiasis.
The verrucose plaque form of leukoplakia is accompanied by roughness, an unusual type of oral mucous membrane. Plaques of various shapes and contours with clear borders rise above the surrounding mucous membrane, the colour of which has not changed. However, unlike the red flat stripper of hyperkeratosis (plaque) is more often single, its location corresponds to the impact of a traumatic factor (acute edge of the tooth, prosthesis, cigarette smoke). The most frequent localization of plaques is the mucous membrane of the corners of the mouth, the sky, the back of the tongue, the red edging of the lips. At palpation of the focus may be observed a small seal. Papuletic elements are absent. Kebner's symptom is negative. In histological study, hyperkeratosis prevails, no acanthosis.
White plaque in pseudomembranous form of candidiasis consists of desquamated cells of epithelium, fibrin, yeast mycelium, bacteria. The film is easily removed by exposing the pinkish-red spot. From the anamnesis reveals prolonged use of antibiotics or corticosteroid drugs, as well as diabetes, hypovitainosis.
Stypical shape
Complaints: burning, soreness, bleeding gums in the area of the front group of teeth of the upper jaw, especially when brushing teeth.
Pathogenesis: inflammatory exudate in its own mucous layer and inflammatory mediators squeeze and irritate the nerve endings.
Duration of the disease: from several weeks to several years.
Efficacy of treatment: treatment is usually carried out for gingivitis or periodontitis (misdiagnosis) and is therefore ineffective. Examination. External examination without changes. The mucous membrane of the alveolar part of the gum in the area of the anterior tooth group of the upper jaw and upper lip is hyperemic, swollen, epithelium is thinned. Erosion is rare. The papules are grayish-white, barely discernible. The mouths of small salivary glands on the mucous membrane of the upper lip are dilated.
Pathogenesis is similar to exudative-hyperemic and erosive- ulcerative forms. Additional research methods for all forms of flattened deprivation. Cytological study: scrape off long-lasting erosive and hyperkeratotic plaques (if malignancy is suspected). The method aims to detect atypical cells.
Bacterioscopic examination: scraping off elements of lesions in the oral mucosa. Aimed at detecting pathogenic bacterial and fungal flora.
Fluorescent Diagnosis: flat shedding papules give a bluish glow on the red edging of the lips and a whitish blue glow on the oral mucous membrane.
Determination of microcurrents: galvanosis. Microcurrents inhibit the action of saliva enzymes, disturb phagocytosis, contribute to sensitizing the mucous membrane, thus provoking the appearance of flattened shingles.
Biochemical study of blood: a quantitative sugar content, liver samples, prothrombin index, etc. There are data on the pathogenetic dependence of flattened shingles on diabetes mellitus, hypertension (Greenspan syndrome) and liver diseases.
Allergological testing: skin samples, laboratory tests (ELISA, RTML, RBT, TDTC, etc.) to detect sensitization to drugs, chemicals, dental materials, food, bacterial agents.
Articles
Sheepskin Treatment
When the diagnosis of red flat is made, the patient is examined for somatic diseases. The gastrointestinal tract should be examined in the first place. It is also necessary to determine the blood sugar content and blood pressure. If a pathology is detected, the patient should be treated by a specialist.
In any form of disease, treatment should be comprehensive, including local and general, which aims to eliminate inflammatory process in the mouth, treatment of concomitant oral pathology, identified common diseases. General treatment of all forms of RFL is the elimination of keratosis, inflammation and normalization of the cornification process of the epithelium, as well as the elimination of intra- and para-focal complications (erythema, erosions, blisters, warts, ulcers).
Necessary hyposensitizing therapy, therapy aimed at increasing the resistance of the body, the elimination of stressful situations. Used pharmacotherapy and physiotherapy, phytotherapy, surgical methods, conducted oral sanitation and dispensary monitoring of patients.
Typical form
Local treatment
- oral hygiene correction;
- oral sanitation;
- elimination of galvanosis, mechanical traumatic factors;
- rational prosthetics;
Local methods of treatment in any form of red flattened lichen precedes and accompanies professional hygiene. Professional hygiene includes: determination of the hygienic state of the mouth, removal of soft and mineralized tooth deposits, teaching the rules of dental care, periodontium, tongue, choice of means and hygiene items, polishing of the tooth surface and remineralization therapy. It is also obligatory to eliminate areas of dental plaque retention (rough surfaces of fillings, restoration of contact points, replacement of wide and deep artificial crowns, irrationally produced dentures, treatment of abnormal position of teeth and abnormal bite, etc.).

The above measures are intended to prevent possible complications and the progression of the disease.
- Epithelizing agents:
- oil solutions of vitamins A and E: retinol acetate oil solution of 3.4%, aevitol, evitol, pumpkin - vitamin A application 2-3 times a day for 15-20 minutes to the lesion area. Application of vitamin A normalizes the function of epithelial cells, prevents the progression of hyperkeratosis, stimulates the regeneration of epithelial cells;
- Aktovegin (gel or ointment), Solkoseril - applications 2 times a day or 1 time in combination with methyluracil ointment;
- Methyluracil ointment - applications;
- Prescription of a gentle diet (except for sour, spicy, hot food), as well as the prohibition of smoking and alcohol.
General treatment
- Sedatives enhance and concentrate the inhibition processes in the cortex, balancing the excitation and inhibition processes. The effect depends on the type of nervous activity, the severity of neurosis. They act soothing, reduce irritability, but unlike tranquilizers do not eliminate the feeling of fear.
- Tincture of valerian, motherwort, peony;
- Novo-Passit 1 h.p. liter 1 g. 3 times a day;
- Glycine 1 ton sublingual 2-3 times a day;
- Antidepressants:
- Azafen - 25 mg 2-3 times a day after meals (course 1-1.5 months);
- Tranquilizers eliminate the feeling of tension, anxiety, fear in neurotic disorders, stressful situations. Suppress the excitability of subcortical areas (limbic system of thalamus, hypothalamus), which are responsible for emotional reactions. Decelerate interaction with the cortex. Interacting with benzodiazoline receptors that are structurally linked to amino acid receptors (GABAs), tranquilizers. Enhance inhibitory processes in brain systems where GABA is the neurotransmitter.
- Phenazepam 0.0005 g
- Siabozone 2 mg
- Relanium 2 mg
- Seduxen 2 mg
- Vitamin therapy: improves metabolic processes, increases the body's resistance. When combined use of vitamins have a stronger and more versatile biological effect, taking part in various biochemical processes.
- provitamin A - Vetoron-T for 1 t after a meal of 1 month);
- Pumpkin - 1 tsp. 30 min. before a meal);
- Aevit - 1 caps. 2 times a day with the course up to one month;
- Milgamma, Riboflavin (vitamins of group B) - 1 dragee 3 times a day course of 1.5 months;
- Nicotinic acid, nicotinamide (vitamins PP) - 0.1 g each. 2-3 times a day for a course of 1 month.
- Immunocorrective therapy to increase the resistance of the mucous membrane of the oral cavity.
- Lycopid - 1mg 2 times a day for 30 minutes before a meal for 14 days;
- Imudon - 6-8 tablets per day sublingually, course 20 days.
- These preparations have immunomodulatory properties, increasing the activity of phagocytes, T- and B-leukocytes, while increasing the bactericidal and cytotoxic activity of phagocytes, stimulating the synthesis of specific antibodies and cytokines.
- Consultation with other specialists (neurologist, gastroenterologist, cardiologist) to detect accompanying pathology.
Exudative-hyperemic form
Local treatment
- Oral sanitation (correction of oral hygiene, treatment of cavities, periodontal tissue diseases, the elimination of electroplating, mechanical trauma factors, prosthetics).
- Pain relief (excitability of sensitive nerve endings is reduced or completely suppressed and excitation of nerve endings is inhibited):
- trimekain solution 3-5%
- 2% lidocaine solution;
- pyromecaine solution 2%;
- anesthesia in oil 5%
- In the form of mouth baths and applications for 3-5 minutes.
- Antiseptics eliminate or reduce the effect of secondary microflora on damaged oral mucosa. Have a bacteriostatic, bactericidal, anti-inflammatory effect, stimulate phagocytosis.
- Hexoral 0.2%
- Corsadil 0.2%
- Chlorhexidine 0.06%
- In the form of mouth baths.
General treatment
- Vitamin therapy
- Milgamma (B1 and B12) - 1 dragee 3 times a day for 1.5 months (has analgesic, anti-allergic effect, increased blood flow, acceleration of regeneration of nervous tissue).
- Nicotinic acid 1% solution (increases blood flow in the capillaries, improves cell metabolism in tissues, promotes collateral circulation) - in the form of injections under the elements of lesion (o.5 - 1.0 ml. N 10;
- Nicotinamide - 0.5 g to 1 tab. 3 times a day course of 1.5 months.
- Compamin (xanthinol nicotinate) - 2 tabs. 3 times a day after meals, as the dose improves, reduced to 1 tab. 3 times a day for a course of 2 months.
- Correction of microcirculation
- Trental - 400 mg. 1 tab. 3 times a day for 1 month (has antispasmodic activity, causes vasodilation, improves microcirculation);
- Ascorutin - 2 tabs. 3 times a day for a course of 1 month. (reduces exudation, increases resistance to orgasm);
- Antihistamine therapy
- Suprastin - 0.025 g 1 tab. 3 times a day course of 14 days;
- Tavegil - 0.001 g 1 tab. 3 times a day for the course of 14 days;
- Claritin - 10 mg. 1 tab. 1 Tab. 1 time per day for the course of 14 days;
- Immunocorrective therapy
- Lycopid - 1mg 3 times a day for 14 days;
- Imudon - 6-8 tablets per day sublingually, course 20 days.
- Treatment of common diseases in specialists.
Erosive ulcer and bullous form
Local treatment
- Oral sanitation
- Oral mucosa pain relief
- trimekain solution 3-5%
- 2% lidocaine solution;
- pyromecaine solution 2%;
- anesthesia in oil 5%
- In the form of mouth baths and applications for 3-5 minutes.
- Antiseptic treatment
- hydrogen peroxide 0.5-1% solution;
- Hexoral 0.2%;
- Corsadil 0.2%;
- chlorhexidine solution 0.06%
- In the form of mouth baths.
- Enzymes
- Lysocyme 0.05% in the form of applications for 15-20 minutes.
- Corticosteroid therapy
- Prednisolon ointment 0.5% - applications for 15-20 min.
- Epithelializing therapy
- oil solutions of vitamin A, rosehip oil, sea buckthorn oil - applications for 15-20 min;
- Caratolin - applications for 15-20 min;
- Jelly-silk, ointment-silk, dental solkoseryl - applications for 15-20 min;
- Aevit - ointment - applications for 15-20 min; Karatolin - applications for 15-20 min;
- Aktovegin - ointment (if prescribed together with Aevit ointment - you can use the scheme: (Aevit - in the morning, Aktovegin - in the evening).
General treatment
- Sedative therapy
- Fnazepam 0.0005 g;
- Cybasone 2 mg;
- Relanium 2 mg;
- Seduxen 2 mg;
- Appointed with a minimum dose of half a tablet overnight;
- Novo-Passit - inwards in 5 ml 3 times daily;
- Vitamin therapy
- Ascorbic acid - 1 g per day;
- Aevit - 1 caps. 2 times a day course 1 month;
- Anti-inflammatory therapy
- Glucocorticosteroids (prednisolone, hydrocortisone, triamcinolone, dexamethasone) inside. Course of treatment 1-2 months on the scheme;
- Diprospan - 1 ml. v/m injection once every 2-4 weeks;
- On the 10th day after the injection of Diprospan prescribe Dalargin for 10 days;
- Delagil (hingamin) - 0.25 g intravenous 10-day course; then injections of Delagil under the elements of lesion in 1.5 ml with 0.5 ml 1% trimecaine;
- Antihistamine therapy
- Suprastin - 0.025 g 1 tab. 3 times a day course of 14 days;
- Tavegil - 0.001 g 1 tab. 3 times a day for the course of 14 days;
- Claritin - 10 mg. 1 tab. 1 Tab. 1 time per day for the course of 14 days;
- Hyposensitizing therapy
- Histaglobulin - p/k in 2-3 ml after 3 days of N 10 (administered with increased content of histamine in the blood);
- Stimulation of tissue exchange
- Solkoceryl - 2ml w/m N 10;
- Immunocorrective therapy
- Lycopid - 1mg 3 times a day for 14 days;
- Imudon - 6-8 tablets per day sublingually, course 20 days;
- Treatment of general diseases;
- Physiotherapeutic treatment (helium-neon laser);
- Cryodestruction (exposure to long-term non-healing erosion by liquid nitrogen).
Hyperkeratotic form
Local treatment
- Surgical treatment (surgical dissection or removal using a laser scalpel).
It is performed if the shape is combined with other forms of flattening.
- Cryodestruction
Conducted by applying liquid nitrogen to plaques to prevent malignization.
General treatment
General treatment is carried out in those forms with which the hyperkeratotic form is combined.
Physiotherapeutic methods of treatment of RFL
For all forms of RFL shows nicotinic acid electrophoresis, which is alternated with vitamin B1 electrophoresis. It is more effective to conduct various courses of electrophoresis on schemes I and II: I - (nicotinic and ascorbic acid), II - vitamin B (and trimecaine) - 20-30 sessions per course.
With forms of RFL with violation of the integrity of the mucous membrane of the oral cavity prescribed means to accelerate epithelization: vacuum - phonophoresis levamizole 0.1%, laser therapy, and then the scheme I and II.
Regardless of the clinical form of the disease at RFL in order to generally affect the body prescribe magnesium electrophoresis, bromine (10% solution) for the cervical zone N 10.
Laser therapy: monochromatic, coherent radiation of low-energy optical quantum generators (lasers) has analgesic, anti-edema, anti-inflammatory effect, accelerates tissue regeneration. The radiation of helium-neon lasers is used with a wavelength of 632 nm.
Prevention of flat stripping
An important factor in the complex of preventive measures is a diet with the exception of irritating food (sour, hot, spicy), as well as the cessation of smoking and alcohol. To prevent relapses and improve the body's protective properties during remission, it is recommended to conduct a course of treatment with compamine, which increases blood flow in the capillaries, improves cell metabolism in tissues, promotes the development of collateral blood circulation. Courses of injection of complamin repeated 2 times a year in combination with taking multivitamins.
Eating errors, stress tend to exacerbate the disease. Cancellation of treatment by a doctor or cessation of treatment by the patient immediately after epithelialization of erosion often leads to exacerbation of the disease.
By: Dr. Samer Jaber